Mesenteric lymphadenitis
Conditions
Overview
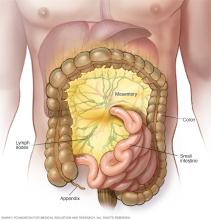
Lymphadenitis is a condition in which the small round or bean-shaped clusters of cells, called lymph nodes, become swollen and inflamed. The swelling can affect the lymph nodes in the membrane that connects the bowel to the wall around the stomach area, called the mesentery. Then the condition is called mesenteric lymphadenitis (mez-un-TER-ik lim-fad-uh-NIE-tis).
An infection in the intestines, such as a virus, is the usual cause of mesenteric lymphadenitis. Also called mesenteric adenitis, the condition mainly affects children and teens.
Mesenteric lymphadenitis can act like appendicitis or a condition in which part of the intestine slides into another part of the intestine, called intussusception. Unlike appendicitis or intussusception, mesenteric lymphadenitis usually clears up on its own.
Symptoms
Possible symptoms of mesenteric lymphadenitis include:
- Pain in the stomach area, often on the lower right side, but the pain can be more spread out.
- General tenderness of the stomach area.
- Fever.
- Enlarged mesenteric lymph nodes.
Depending on what's causing the condition, symptoms also might include:
- Diarrhea.
- Nausea and vomiting.
When to see a doctor
Pain in the stomach area is common in children and teens. So it can be hard to know when to seek medical advice.
Call a healthcare professional right away for a child who has:
- Sudden, severe pain in the stomach area.
- Stomach area pain with fever.
- Stomach area pain with diarrhea or vomiting.
- Tenderness to touch of the stomach area.
- Bloody or maroon-colored stool.
Also, call a healthcare provider for a child who has pain in the stomach area that doesn't get better in a short time and who also:
- Has a change in bowel habits.
- Has a loss of appetite.
- Is not able to sleep.
Causes
The most common cause of mesenteric lymphadenitis is a viral infection, such as gastroenteritis. Gastroenteritis is often called stomach flu. This infection causes inflammation and swelling in the lymph nodes in the thin tissue that attaches the intestine to the back of the wall around the stomach area, called mesentery.
Other causes of mesenteric lymphadenitis include bacterial infection, inflammatory bowel disease and lymphoma.
Risk factors
Any infection that causes inflammation and swelling in the lymph nodes in the tissue that attaches the bowel to the abdominal wall increases the risk of mesenteric lymphadenitis.
Conditions that raise the risk of mesenteric lymphadenitis include:
- Viral or bacterial gastroenteritis.
- Inflammatory bowel disease.
- Lymphoma.
Diagnosis
Diagnosing mesenteric lymphadenitis involves taking a medical history and doing an exam. Tests might include:
- Blood tests. Certain blood tests can help show if there's an infection and what type of infection it is.
- Imaging studies. An ultrasound of the stomach area is often used to diagnose mesenteric lymphadenitis. A CT scan of the stomach area also might be used.
Treatment
Mild cases of mesenteric lymphadenitis and those caused by a virus usually go away on their own. Full recovery can take four weeks or more.
For treatment of fever or pain, consider giving your child infants' or children's over-the-counter fever and pain medications such as acetaminophen (Tylenol, others) or ibuprofen (Advil, Motrin, others). They're safer than aspirin.
Use caution when giving aspirin to children or teenagers. Though aspirin is approved for use in children older than age 3, children and teenagers recovering from chickenpox or flu-like symptoms should never take aspirin. This is because aspirin has been linked to Reye's syndrome, a rare but potentially life-threatening condition, in such children.
Antibiotics might be prescribed for a moderate to severe bacterial infection.
Lifestyle and home remedies
For symptoms of mesenteric lymphadenitis, have your child:
- Get plenty of rest. Enough rest can help your child recover.
- Drink fluids. Liquids help prevent loss of body fluids, called dehydration, from fever, vomiting and diarrhea.
- Apply moist heat. A warm, moist washcloth applied to the stomach area can help ease discomfort.
- Eat a liquid diet in small amounts. For example, eat broth or chicken noodle soup.
Preparing for an appointment
If your child has symptoms of mesenteric lymphadenitis, make an appointment with a healthcare professional. Here's some information to help you get ready for your appointment.
What you can do
Make a list of:
- Your child's symptoms, including symptoms that don't affect the stomach, and when they began. If possible, take your child's temperature several times before your appointment and record the results.
- Your child's key medical information, including other health conditions. Also list all medicines, vitamins and supplements your child takes, including doses. And take a record of your child's recent vaccinations.
- Questions to ask your healthcare professional.
For possible mesenteric lymphadenitis, some questions to ask include:
- What's the likely cause of my child's condition? Are there other possible causes?
- What tests does my child need?
- Is my child likely to have complications from this condition?
- Does my child need treatment? If this is due to an infection, should my child take antibiotics?
- What can I do to make my child more comfortable? Are there foods my child shouldn't eat?
- What symptoms should prompt me to call you while my child is recovering?
- Is my child's illness catching?
- When can my child return to school?
What to expect from your doctor
Your child's healthcare professional might ask:
- Where is the pain?
- Has the pain moved from one part of your child's stomach to another part?
- How bad is the pain? Does your child cry with pain or insist on lying down?
- What makes the pain feel worse?
- What helps relieve the pain?
- Has your child had problems like this before?
- Do other children in your family or at school or at child care have symptoms like your child's?
© 1998-2026 Mayo Foundation for Medical Education and Research(MFMER). All rights reserved. Terms of Use
