Retinoblastoma
Conditions
Overview
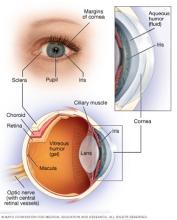
Retinoblastoma is a kind of eye cancer that starts as a growth of cells in the retina. The retina is the light-sensitive lining on the inside of the eye.
The retina is made up of nerve tissue that senses light as it comes in through the front of the eye. The light causes the retina to send signals to the brain. The brain interprets the signals as images.
Retinoblastoma happens most often in young children. It's usually diagnosed before age 2. It most often affects one eye. Sometimes it happens in both eyes.
There are several treatments for retinoblastoma. For most children, treatment doesn't require removing the eye to get rid of the cancer. The outlook for children diagnosed with retinoblastoma is quite good.
Symptoms
Retinoblastoma signs and symptoms include:
- A white color in the center circle of the eye when light is shone in the eye. It might show up in flash photos.
- Eye redness.
- Eye swelling.
- Eyes that seem to be looking in different directions.
- Vision loss.
When to see a doctor
Make an appointment with a doctor or other healthcare professional if you notice any changes to your child's eyes that concern you.
Causes
Retinoblastoma is caused by changes inside the cells in the eye. It's not always clear what causes the changes that lead to this eye cancer.
Retinoblastoma starts when cells in the eye get changes in their DNA. A cell's DNA holds the instructions that tell the cell what to do. In healthy cells, the DNA gives instructions to grow and multiply at a set rate. The instructions also tell the cells to die at a set time. In cancer cells, the DNA changes give different instructions. The changes tell the cancer cells to make many more cells quickly. Cancer cells can keep living when healthy cells would die. This causes too many cells.
In retinoblastoma, this growth of cells happens in the retina. The retina is the light-sensitive lining on the inside of the eye. The retina is made up of nerve tissue that senses light as it comes in through the front of the eye. The light causes the retina to send signals to the brain. The brain interprets the signals as images.
As the cancer cells build up in the retina, they can form a mass, called a tumor. The tumor can grow to invade and destroy healthy body tissue. In time, cancer cells can break away and spread to other parts of the body. When cancer spreads, it's called metastatic cancer. Retinoblastoma rarely spreads, especially if it's found early.
For most instances of retinoblastoma, it's not clear what causes the DNA changes that lead to cancer. However, it's possible for children to inherit DNA changes from their parents. These changes can increase the risk of retinoblastoma.
Risk factors
Risk factors for retinoblastoma include:
- Young age. Retinoblastoma is most common in very young children. It's typically diagnosed by age 2. Retinoblastoma that happens later in life is very rare.
- DNA changes that run in families. DNA variations that increase the risk of retinoblastoma can be passed from parents to children. Children with these inherited DNA changes tend to get retinoblastoma at a younger age. They also tend to have retinoblastoma in both eyes.
Complications
Children with retinoblastoma can develop complications.
Cancer that comes back
After treatment, there is a risk that the cancer might come back in the eye or near it. For this reason, your child's healthcare team will create a plan of follow-up appointments. Your child's follow-up plan will depend on the treatments your child received. A typical plan might involve eye exams every few months for the first few years after treatment.
Increased risk of other cancers
Children with the form of retinoblastoma that can run in families may have a higher risk of getting other kinds of cancer.
The risk of these cancers is increased:
- Bone cancer.
- Bladder cancer.
- Breast cancer.
- Hodgkin lymphoma.
- Lung cancer.
- Melanoma.
- Pineoblastoma.
- Soft tissue sarcoma.
Your child's healthcare team might recommend tests to screen for these other types of cancers.
Prevention
There's no way to prevent retinoblastoma.
Some retinoblastomas are caused by DNA changes that run in families. If retinoblastoma runs in your family, tell your healthcare professional. Together you might consider genetic testing to look for variations in your DNA that increase the risk of retinoblastoma. Your health professional might refer you to a genetic counselor or other healthcare professional trained in genetics. This person can help you decide whether to undergo genetic testing.
If your children have an increased risk of retinoblastoma, care can be planned to manage that risk. For instance, eye exams may begin soon after birth. That way, retinoblastoma may be diagnosed very early. These screening tests could find the cancer when it is small and has a greater chance of being cured.
If you haven't had children, but are planning to, talk with your healthcare team about your family history of retinoblastoma. Genetic testing might help you and your partner understand whether there is a risk of passing DNA variations to your future children. Your healthcare team may have options to help you manage this risk.
Diagnosis
Retinoblastoma diagnosis often starts with an eye exam. Imaging tests can help show the size of the cancer.
Eye exam
A healthcare professional carefully examines your child's eyes during an eye exam. This might involve testing your child's vision and using a special light to look inside the eye. Sometimes very young children find it hard to hold still for a thorough eye exam. Your healthcare team might recommend medicine to put the child in a sleep-like state so the exam can be completed. The results of the eye exam give your healthcare team clues about what's causing your child's symptoms.
Imaging tests
Imaging tests make pictures of the inside of the body. For retinoblastoma, imaging tests are used to look at the eye and the area around it. The images might show the size of the cancer and whether it has grown beyond the eye. Imaging tests may include ultrasound and MRI, among others.
Genetic testing
Genetic testing uses a sample of blood or saliva to look for variations in the DNA. Genetic testing for retinoblastoma looks for variations in a part of the DNA called the RB1 gene.
Everyone with retinoblastoma has variations in the RB1 gene in their cancer cells. But some children with retinoblastoma have the RB1 gene variations in all of the cells in their bodies. This can happen if parents pass DNA variations to their child. The variations also can happen if something changes the RB1 gene as the child develops in the womb.
If genetic testing shows your child has variations in the RB1 gene in all of the cells in the body, this helps the healthcare team plan your child's treatment. Having variations in the RB1 gene in all of the cells also raises the risk of other kinds of cancer. Screening tests can help watch for those other kinds of cancer.
Treatment
Common retinoblastoma treatments include chemotherapy, cold therapy and laser therapy. Radiation therapy may be another option. Surgery to remove the eye can treat retinoblastoma, but it's only used in certain situations.
Which treatment is best for your child's retinoblastoma depends on several factors. These factors include the size and location of the cancer, and whether cancer has spread beyond the eye. Your healthcare team also considers your child's overall health and your own preferences.
Chemotherapy
Chemotherapy treats cancer with strong medicines. It's often the first treatment for retinoblastoma. Other treatments might be needed after chemotherapy to kill any cancer cells that remain.
Types of chemotherapy used to treat retinoblastoma include:
- Chemotherapy that travels through the entire body. Chemotherapy medicines can be given through a vein or in pill form. These medicines travel throughout the body to kill cancer cells. Giving the medicines in this way is called systemic chemotherapy. Treatment is typically given monthly for several months.
- Chemotherapy put into an artery near the cancer. Chemotherapy medicines can be put into an artery near the eye. To get the medicine to the right place, a thin tube is inserted through the skin and into an artery in the groin. The tube is advanced through the body until it gets near the eye. Then the medicine is released through the tube. Giving the medicine in this way is called intra-arterial chemotherapy. It lets the healthcare team give the medicine directly to the eye. Treatment is typically done monthly for a few months.
- Chemotherapy injected in the eye. Sometimes chemotherapy medicines are injected in the eye with a needle. This way of giving the medicines is called intravitreal chemotherapy. It's typically used after other kinds of chemotherapy. It might be used when some cancer remains after other treatments or when the cancer comes back.
Cold therapy
Cold therapy, also called cryotherapy, uses extreme cold to damage cancer cells. It's typically used after chemotherapy to kill any cancer cells that are left. For very small retinoblastomas, cryotherapy might be the only treatment needed.
During cryotherapy, a very cold instrument is placed on the eye. This causes the nearby cells to freeze. Once the cells freeze, the instrument is removed. This causes the cells to thaw. This process of freezing and thawing is repeated a few times in each cryotherapy session.
Laser therapy
Laser therapy uses a laser light to heat up and damage the cancer cells. The medical term for this procedure is transpupillary thermotherapy. It's typically used after chemotherapy to kill any cancer cells that are left. For very small retinoblastomas, laser therapy might be the only treatment needed. Treatments are typically repeated every few weeks until there are no signs of active cancer in the eye.
Radiation therapy
Radiation therapy treats cancer with powerful energy. Types of radiation therapy used in treating retinoblastoma include:
-
Placing a radiation device on the eye. A device that emits radiation can be placed on the eye. This kind of radiation is called plaque radiotherapy. It uses a small disk that holds radioactive material. The disk is stitched into place on the eye and left for a few days while it slowly gives off radiation to the cancer.
Placing radiation near the cancer reduces the chance that treatment will affect healthy tissues outside the eye. This type of radiation therapy is typically used for cancers that don't respond to chemotherapy.
-
Using a machine to aim radiation at the eye. Radiation can be given to the retinoblastoma using a machine that aims energy beams at the cancer. The energy beams can be made of X-rays, protons or other kinds of radiation. As your child lies on a table, the machine moves around your child, delivering the radiation. This kind of radiation is called external beam radiation. Treatments typically happen daily for several weeks.
External beam radiation can cause side effects if the radiation beams reach the delicate areas around the eye, such as the brain. For this reason, external beam radiation is typically reserved for children with retinoblastoma that extends beyond the eye.
Eye removal surgery
When other treatments haven't worked or when the retinoblastoma is too large to be treated by other methods, surgery to remove the eye may be used. In these situations, eye removal may help prevent the spread of cancer to other parts of the body. Eye removal surgery for retinoblastoma includes:
- Surgery to remove the affected eye. Surgery to remove the eye is called enucleation. Surgeons disconnect the muscles and tissue around the eye and remove the eyeball. A portion of the optic nerve, which extends from the back of the eye into the brain, also is removed.
-
Surgery to place an eye implant. Immediately after the eyeball is removed, the surgeon places a special ball in the eye socket. The ball is called an implant. The muscles that control eye movement are sometimes attached to the implant.
After your child heals, the eye muscles will adapt to the implant. It may move just as the natural eye did. However, the implant can't see.
-
Fitting an artificial eye. Several weeks after surgery, a custom-made artificial eye can be placed over the eye implant. The artificial eye can be made to match the appearance of your child's healthy eye.
The artificial eye sits behind the eyelids. As your child's eye muscles move the eye implant, it will appear that your child is moving the artificial eye.
Risks of surgery include infection and bleeding. Removing an eye will affect your child's vision. Most children adapt to the vision changes over time. Your child will need to take extra caution to protect the healthy eye. For example, after surgery, children should wear protective glasses or sport goggles while playing sports.
Clinical trials
Clinical trials are studies to test new treatments and new ways of using existing treatments. While clinical trials give your child a chance to try the latest in retinoblastoma treatments, they can't guarantee a cure.
Ask your child's doctor whether your child is eligible to participate in clinical trials. Your child's doctor can discuss the benefits and risks of enrolling in a clinical trial.
Coping and support
When your child is diagnosed with cancer, it's common to feel a range of emotions. Parents sometimes say they felt shock, disbelief, guilt or anger after their child's diagnosis. Everyone finds his or her own way of coping with stressful situations. Until you find what works for you, you might try to:
Gather all the information you need
Find out enough about retinoblastoma to feel comfortable making decisions about your child's care. Talk with your child's healthcare team. Keep a list of questions to ask at the next appointment.
Ask your healthcare team where you can learn more about retinoblastoma. Good places to start include the websites for the National Cancer Institute and the American Cancer Society.
Organize a support network
Find friends and family who can help support you as a caregiver. Loved ones can accompany your child to appointments or sit by the bedside in the hospital when you can't be there.
When you're with your child, your friends and family can help out by spending time with your other children or helping around your home.
Take advantage of resources for kids with cancer
Seek out special resources for families of kids with cancer. Ask your clinic's social workers about what's available.
Support groups for parents and siblings put you in touch with people who might understand what you're feeling. Your family may be eligible for summer camps, temporary housing and other support.
Maintain your routine as much as possible
Small children can't understand what's happening to them as they undergo cancer treatment. To help your child cope, try to maintain a usual routine as much as possible.
Try to arrange appointments so that your child can have a set nap time each day. Have routine mealtimes. Allow time for play when your child feels up to it. If your child must spend time in the hospital, bring items from home that will help your child feel more comfortable.
Ask your healthcare team about other ways to comfort your child during treatment. Some hospitals have recreation therapists or child life specialists who can share advice and resources.
Preparing for an appointment
Start by making an appointment with your child's doctor or other healthcare professional if your child has any signs or symptoms that worry you. If an eye problem is suspected, you may be referred to a doctor who diagnosis and treats eye conditions. This doctor is called an ophthalmologist. If retinoblastoma is suspected, your child may see a doctor who specializes in treating eye cancer. This doctor is called an ocular oncologist.
Because appointments can be brief, it's a good idea to be prepared. Here's some information to help you get ready.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your child's diet.
- Write down any symptoms your child is experiencing, including any that may seem unrelated to the reason for which you scheduled the appointment.
- Write down key personal information, including any major stresses or recent changes in your child's life.
- Make a list of all medications, vitamins or supplements your child is taking.
- Take a family member or friend along. Sometimes it can be difficult to remember the information provided during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your child's doctor.
Prepare a list of questions to help you make the most of the time with your child's healthcare professional. List your questions from most important to least important in case time runs out. For retinoblastoma, some basic questions to ask include:
- What kinds of tests does my child need?
- What is the best course of action?
- What are the alternatives to the primary approach that you're suggesting?
- Should my child see a specialist?
In addition to the questions that you've prepared, don't hesitate to ask other questions during your appointment.
What to expect from your child's doctor
Your child's healthcare professional is likely to ask you a number of questions. Be ready to answer some questions about your child's health and symptoms, such as:
- Has your child ever had cancer before?
- Does your family have a history of cancer?
- Does your child have any siblings? How old are they? Have they ever had an eye exam?
- When did your child begin experiencing symptoms?
- Have your child's symptoms been continuous or occasional?
- How severe are your child's symptoms?
- What, if anything, seems to improve your child's symptoms?
- What, if anything, appears to worsen your child's symptoms?
© 1998-2026 Mayo Foundation for Medical Education and Research(MFMER). All rights reserved. Terms of Use
