Brain metastases
Conditions
Overview
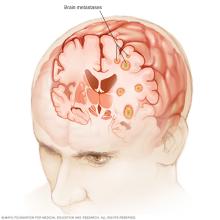
Brain metastases are cancers that have spread to the brain from another part of the body. They are sometimes called brain mets. They also are known as secondary brain tumors.
Secondary brain tumors are cancers that started somewhere else in the body and then spread to the brain. They keep the name of the original cancer, for example, metastatic breast cancer. Secondary brain tumors are different from primary brain tumors, which begin in the brain itself.
Any cancer can spread to the brain. The most common cancers that spread to the brain include lung, breast, colon, kidney and melanoma.
Brain metastases can form one or multiple tumors in the brain. As the tumors grow, they may cause swelling and put pressure on surrounding brain tissue. This can lead to symptoms such as headache, personality changes, confusion, seizures, vision changes, trouble speaking, numbness, weakness or issues with balance.
Treatment for people whose cancer has spread to the brain depends on many factors, including the type of cancer, the number and location of brain metastases, and overall health. Treatment may include surgery, radiation therapy, immunotherapy, targeted therapy or chemotherapy. Other treatments may be used to help manage symptoms caused by brain metastases.
The outlook for people with brain metastases can be very different from person to person. It depends on things such as where the cancer started, how many brain metastases there are, whether the cancer is controlled elsewhere in the body and overall health.
Brain metastases, also called brain mets or secondary brain tumors, occur when cancer spreads from another part of the body to the brain.
Brain metastases are classified based on where cancer cells spread within the central nervous system. The two main patterns of spread are parenchymal metastases and leptomeningeal metastases. These patterns affect different parts of the brain and spinal cord and may require different approaches to diagnosis and treatment.
Parenchymal metastases
Parenchymal metastases occur when cancer spreads from another part of the body into the brain tissue itself. These form discrete tumors within the brain. A person may have one tumor or several tumors located in different areas.
Parenchymal metastases are the most common form of brain metastasis.
Leptomeningeal metastases, also called leptomeningeal disease
Leptomeningeal metastases, also called leptomeningeal disease (LMD) or neoplastic meningitis, occur when cancer cells spread to the thin layers of tissue and the cerebrospinal fluid that surround the brain and spinal cord.
Instead of forming a single mass, cancer cells spread along the surface of the brain and spinal cord and within the fluid that circulates around them. This pattern of spread can affect multiple areas of the nervous system.
Symptoms
Symptoms of brain metastases depend on where cancer has spread within the brain or surrounding tissues, how large the affected areas are, and how quickly they are growing. Symptoms are not determined by the original cancer type, such as lung or breast cancer. Instead, they relate to which parts of the nervous system are involved.
Some people develop symptoms gradually, while others notice symptoms more quickly.
Symptoms of parenchymal metastases
Parenchymal metastases form tumors within the brain tissue. Symptoms usually relate to the specific area of the brain where the tumor is located.
Symptoms may include:
- Headache, which may become more frequent or more severe over time and may occur with nausea or vomiting.
- Changes in thinking or behavior, such as confusion, difficulty concentrating or increasing memory issues.
- Seizures, even in people who have never had seizures before.
- Weakness or numbness, often affecting one side of the body.
- Vision changes, such as blurred vision, double vision or loss of part of the visual field.
- Difficulty speaking or understanding language.
- Balance or coordination issues.
Symptoms of leptomeningeal metastases
Leptomeningeal metastases involve cancer cells spreading within the fluid and thin tissues that surround the brain and spinal cord. Because this spread can affect multiple areas of the nervous system at the same time, symptoms may be more widespread.
Symptoms may include:
- Headaches.
- Nausea and vomiting.
- Vision changes, such as blurred vision or double vision.
- Facial weakness or numbness.
- Hearing loss.
- Difficulty swallowing.
- Confusion or changes in thinking or behavior.
- Weakness or loss of feeling in the arms or legs.
- Back or neck pain that may spread into the arms or legs.
- Difficulty with bowel or bladder control.
- Changes in alertness.
- Seizures.
When to see a doctor
Make an appointment with your healthcare professional if you have new, ongoing or worsening symptoms that concern you, especially symptoms related to headaches, seizures, thinking, vision, balance or weakness.
If you have been treated for cancer in the past, tell your healthcare professional about your cancer history, even if treatment ended years ago. New neurological symptoms in someone with a history of cancer should be checked.
Causes
Brain metastases occur when cancer cells break away from where they first formed in the body and spread to the brain. The cancer cells usually travel through the bloodstream. In some cases, they may travel through the lymphatic system — a network of vessels and lymph nodes that helps drain fluid and support the immune system — before reaching the brain.
Cancer that spreads from its original location keeps the name of the original cancer. This original cancer is called the primary cancer. For example, cancer that spreads from the breast to the brain is called metastatic breast cancer, not brain cancer.
Risk factors
Any type of cancer can spread to the brain. However, some cancers are more likely to spread than others. These include:
- Lung cancer.
- Breast cancer.
- Colon cancer.
- Kidney cancer.
- Melanoma.
Many other cancers also can spread to the brain, although this happens less often. These include cancers of the liver, ovary, thyroid, pancreas, gastroesophageal region and uterus, as well as some blood cancers. While brain metastases are less common with these cancers, they are still possible and may cause similar symptoms.
Some cancers are unlikely to spread to the brain. These include nonmelanoma skin cancers, such as basal cell carcinoma, and most squamous cell carcinomas of the skin. Other rare cancers, such as Merkel cell carcinoma, can spread beyond the skin. But a spread to the brain is not common.
Cancer that has spread to the spine or spinal cord also may spread to other parts of the nervous system, including the brain, depending on the cancer type and how advanced it is.
Diagnosis
A diagnosis of brain metastases usually begins with a review of symptoms and medical history, including whether someone has been treated for cancer in the past.
If brain metastases are suspected, tests are used to look for tumors in the brain. Sometimes, tests are used to confirm the type of cancer involved.
Tests and procedures used to diagnose brain metastases may include:
- Neurological exam. A healthcare professional checks how well the nervous system is working. This may include testing thinking, speech, vision, hearing, balance, coordination, strength, sensation and reflexes.
-
Imaging tests. Imaging tests create pictures of the brain. Brain MRI is the main test used to diagnose brain metastases. MRI can help show the number, size and location of tumors in the brain. Contrast material is often given through a vein during this test to make tumors easier to see. MRI is very sensitive for finding brain metastases.
Other imaging tests may include computerized tomography (CT) and positron emission tomography (PET). Brain CT scans may be used in urgent situations or when MRI is not available. PET scans are sometimes used to look for cancer elsewhere in the body, but they are not usually the main test for finding brain metastases.
- Biopsy. In some cases, a procedure may be done to remove a small sample of tissue for testing in a lab. A brain biopsy may be done with a needle or during surgery, especially if the diagnosis is not clear or the original cancer is not known.
Can a PET scan show brain metastases?
PET scans can sometimes show brain metastases, but they are not usually the best test for finding cancer in the brain. MRI is more sensitive and is typically used to diagnose brain metastases. PET scans are used more often to look for cancer elsewhere in the body.
What do brain metastases look like on an MRI scan?
On an MRI scan, brain metastases usually appear as one or more areas of unusual tissue in the brain. MRI helps show the number, size and location of brain metastases and whether there is swelling in nearby brain tissue. A contrast is often used to make brain metastases easier to see.
Are brain metastases considered stage 4 cancer?
In many cancers, brain metastases are considered advanced disease. This is often called stage 4 cancer because the cancer has spread to a distant part of the body.
However, cancer staging rules are different for each type of cancer. Whether brain metastases are labeled stage 4 depends on where the cancer started and how that cancer is staged.
Treatment
Treatment for brain metastases can help ease symptoms, slow tumor growth and extend life. Even with successful treatment, brain metastases may return. Ongoing follow-up care with your healthcare team is important.
Treatments will depend on factors such as the type of cancer; the number, size and location of brain metastases; symptoms; overall health; and personal treatment goals.
Medicines to control symptoms
Medicines can help control symptoms of brain metastases and make you more comfortable. Options might include:
- Steroids. These medicines also are called corticosteroids. They may reduce swelling in the brain caused by brain metastases. This can help relieve symptoms such as headache, nausea and weakness.
- Antiseizure drugs. If you're having seizures, these medicines may help control them. They are not typically used unless someone has had a seizure.
Surgery
Surgery may be an option if a brain metastasis is in a location that can be safely reached, and surgery fits into the overall cancer care plan. During brain tumor surgery, the surgeon removes as much of the tumor as possible. Surgery may help relieve symptoms. In some cases, it may help confirm the diagnosis. Surgery is usually combined with other treatments.
Advances in brain surgery have improved safety over time. However, risks may include:
- Difficulty thinking.
- Difficulty with movement.
- Issues with speech.
- Numbness or weakness in the face, arms or legs.
- Infection.
- Bleeding.
The risks also depend on where the tumor is located in the brain, as well as your overall health. You may want to discuss your individual risks with your healthcare team.
Radiation therapy
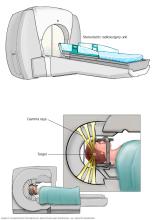
Radiation therapy treats cancer with powerful energy beams. The energy can come from X-rays, protons or other sources. During radiation therapy, you lie on a table while a machine moves around you. The machine directs radiation to targeted areas in the brain to destroy cancer cells.
Radiation therapy for brain metastases may include one or both of the following:
-
Whole-brain radiation therapy. Whole-brain radiation treats the entire brain to target cancer cells. Treatment is usually given over 10 to 15 sessions across 2 to 3 weeks.
Side effects may include fatigue, nausea, skin reaction, headache and hair loss. Long-term, whole-brain radiation may cause decline in thinking and memory. Techniques such as avoiding the hippocampus during treatment and using certain medicines may help lower this risk in some people.
-
Stereotactic radiosurgery. Stereotactic radiosurgery (SRS) is a highly focused form of radiation therapy. It also is called stereotactic radiotherapy. SRS delivers radiation from many angles to precisely target brain metastases while limiting damage to nearby healthy tissue. Treatment may be given in one session or a small number of sessions.
Healthcare professionals use 3D planning to make the treatment as exact as possible and limit damage to healthy parts of the brain.
Side effects may include nausea, headache and fatigue. The risk of thinking and memory decline after SRS is thought to be less than with whole-brain radiation.
Advances in radiation therapy have improved the understanding of how these treatments affect survival, brain function and quality of life. Decisions about radiation therapy are based on factors such as the number of brain metastases, other treatments being used and the likelihood that cancer will return.
Medicines
In some situations, medicines may be used to treat cancer throughout the body and may also help treat brain metastases. Whether these medicines help in the brain depends on where the cancer started, the type of medicine used and individual factors. Options may include:
- Chemotherapy. Chemotherapy uses medicines to kill or slow the growth of cancer cells. Some chemotherapy medicines have limited ability to reach tumors in the brain, while others may be more effective. Chemotherapy is often given through a needle in a vein, though some medicines are taken as pills.
- Targeted therapy. Targeted therapy uses medicines that focus on specific changes in cancer cells. Some targeted therapies can be effective against brain metastases, depending on the type of cancer and the genetic features of the tumor.
- Immunotherapy. Immunotherapy uses medicines that help the body's immune system find and attack cancer cells. Some immunotherapy medicines can help control brain metastases in certain cancers.
Rehabilitation after treatment
Brain metastases can affect areas of the brain that control movement, speech, vision and thinking. Because of this, rehabilitation may be an important part of recovery. A healthcare professional may recommend one or more of the following therapies:
- Physical therapy. Physical therapists can help improve strength, coordination, and the ability to move safely and maintain balance.
- Occupational therapy. Occupational therapists can help with daily activities, such as dressing, bathing and returning to work or other routines.
- Speech therapy. Speech-language pathologists can help if there are problems with speaking, understanding language or swallowing.
- Cognitive rehabilitation therapy. This type of therapy may help with problems related to memory, attention, thinking skills or word finding.
Can brain metastases be cured?
It's uncommon that cancer that has spread to the brain can be cured. Treatments can often slow the growth of brain metastases, relieve symptoms and sometimes shrink tumors for months to years. But a lasting cure is rare and depends on factors such as the type of primary cancer, how much cancer is elsewhere in the body and how the cancer responds to treatment.
Palliative care
Palliative care focuses on helping people with serious illnesses feel better. It's also called supportive care. For people with brain metastases, palliative care can help manage pain and other symptoms.
Palliative care is provided by a team of healthcare professionals. This can include doctors, nurses and other specially trained professionals. The goal is to improve quality of life for both the person receiving care and the person's family.
Palliative care can happen at the same time as treatments such as surgery, radiation therapy or chemotherapy.
Prognosis is an overall estimate of how a disease may affect someone and how the disease may respond to treatment.
The prognosis for people with brain metastases varies widely. It depends on things such as where the cancer started, how many brain metastases there are, whether the growth of the cancer is controlled, overall health and how well treatments work.
Within the first year after diagnosis
Studies show that survival after a diagnosis of brain metastases is most often measured in months, though some people live a year or longer.
Outcomes have improved for some people because of better treatment options, such as stereotactic radiosurgery, targeted therapy and immunotherapy.
How likely someone is to live a year depends heavily on the type of primary cancer, how much cancer is elsewhere in the body and how the cancer responds to treatment.
Long-term prognosis and survival
Five-year survival is not common in general for people with brain metastases. It's possible to live for several years, especially if cancer has spread to only a few places and responds well to treatment.
Because people respond to cancer and treatment differently, a single statistic on how long people live after diagnosis cannot predict what will happen to any one person.
Outlook by primary cancer type
Outlook is a broad way of talking about what may happen in the future, including how someone might do with treatment.
Outlook for brain metastases can vary depending on the type of cancer that spread to the brain and how well that cancer responds to treatment. Many people look for information about life expectancy or survival when a specific cancer, such as lung cancer or melanoma, has spread to the brain.
Some cancers are linked to a better outlook for some people, including:
- Breast cancer, especially when it responds well to available treatments.
- Non-small cell lung cancer with certain genetic changes that can be treated with targeted therapy.
- Melanoma, because of advances in immunotherapy and targeted therapy.
Cancers that often have a more limited outlook include:
- Small cell lung cancer, which tends to spread early and grow quickly.
- Cancers that are widespread elsewhere in the body and do not respond well to treatment.
- Leptomeningeal disease, which is harder to treat than tumors located within the brain tissue.
Even within the same cancer type, outlook can vary widely depending on how much cancer is present, overall health and how well treatment works.
Support and planning
Prognosis is only one part of care planning. Even when survival is limited, treatments can often relieve symptoms, help people keep doing daily activities for as long as possible and improve quality of life.
Palliative care teams can help manage your symptoms and support decision-making at every stage of illness. Your care team can explain what the likely goals of treatment are for your situation and help you and your family plan care that matches your priorities.
What causes death in people with metastatic brain cancer?
The cause of death in people with advanced brain metastases often is cancer that continues to grow in the brain or elsewhere in the body. As brain metastases grow, pressure in the skull can increase. This can worsen thinking or alertness. It can cause weakness, trouble breathing or other serious neurological issues that can no longer be controlled.
When cancer spreads to the lining of the brain and spinal cord, called leptomeningeal disease, issues with thinking, movement, breathing or alertness often worsen over time and can eventually become life-threatening. How this happens varies from person to person and depends on many factors.
What should someone expect in the final stages of brain cancer metastasis?
In the final stages of brain cancer metastasis, symptoms often continue to worsen. People may become more confused or sleepy, feel weaker, or have trouble swallowing or breathing. They may have difficulty moving or communicating. They may have seizures.
At this stage, care usually focuses on comfort, easing symptoms and supporting quality of life. Palliative care and hospice teams can help manage symptoms and provide support for both the person and the family. How this stage looks and how long it lasts varies from person to person and depends on the type of cancer, overall health and treatments used.
Alternative medicine
No complementary or alternative therapies have been shown to treat or cure brain metastases. However, integrative medicine may help some people cope with the stress of cancer and manage side effects of cancer treatment.
Integrative medicine approaches that may be used alongside standard cancer care include:
- Acupuncture.
- Art therapy.
- Massage.
- Meditation.
- Music therapy.
- Physical activity.
- Relaxation exercises.
- Yoga.
- Nutrition support, such as guidance from a registered dietitian.
Some approaches may not be safe for everyone or may interfere with cancer treatment. Talk with your healthcare professional before trying integrative therapies.
Coping and support
Coping with brain metastases involves accepting the news that your cancer has spread beyond its original site.
Cancer that has spread can be difficult to cure. Someone with a single brain metastasis has a better chance of long-term survival than does someone with multiple metastatic tumors. Your healthcare team works to reduce your pain and help you continue your daily activities.
With time you'll find ways to cope with the stress and uncertainty of cancer. Until then, you may find that it helps to:
- Learn about brain metastases. Ask your healthcare professional for details of your cancer. Ask about the type, treatment options and your prognosis. Ask for good sources of up-to-date information.
- Be aware of possible limits on driving. Ask your healthcare professional if it's OK for you to drive. The answer may depend on whether your neurological exam shows that your judgment and reflexes have not been affected and whether you have seizures.
- Express your feelings. Find an activity that allows you to write or talk about your emotions. That may include writing in a journal, talking to a friend, counselor or chaplain, or joining a support group. Ask your healthcare professional about support groups in your area.
- Come to terms with your illness. If treatment isn't helping, you and your family may want to talk with your healthcare team about end-of-life care options, such as hospice.
Preparing for an appointment
Make an appointment with your healthcare professional if you have any symptoms that worry you. Tell your health professional if you've been treated for cancer before, even if it was many years ago.
If you're diagnosed with brain metastases, you likely will be referred to one or more of the following healthcare professionals:
- A neuro-oncologist, who specializes in brain metastases.
- A neurologist, who treats conditions of the nervous system.
- A radiation oncologist, who treats brain tumors with radiation.
- A neurosurgeon, who performs surgery on brain tumors.
Appointments can be brief, and there's a lot to discuss. It's a good idea to be prepared. Here's how to help get ready and what to expect:
What you can do
- Be aware of any pre-appointment rules. When you make the appointment, ask if there's anything you need to do in advance, such as change your diet.
- Write down your symptoms, even those that may not seem related to why you scheduled the appointment. Note how long you've had these symptoms and what makes them worse or better.
- List key personal information, including any major stresses or recent life changes.
- Make a list of all medications, vitamins or supplements that you're taking. Include doses.
- Consider taking a family member or friend along. Sometimes it can be difficult to remember all the information provided during an appointment. Someone who comes with you may remember details you missed or forgot.
- Write down questions to ask your healthcare professional.
Writing a list of questions can help you make the most of your time with your healthcare professional. For brain metastases, some basic questions to ask include:
- What's the most likely cause of my symptoms?
- Are there other possible causes for my symptoms?
- What kinds of tests do I need?
- What treatments are available, and which do you recommend?
- What are the possible side effects of each treatment?
- How will treatment affect my daily life?
- How long will the treatment last?
- What's my prognosis?
- What experimental treatments or clinical trials are available to me?
- I have these other health conditions. How will they affect my treatment?
- Is there a generic alternative to the medicine you're prescribing?
- Do you have any brochures or other printed material that I can take with me? What websites do you recommend?
- If you had a friend or loved one in my situation, what advice would you give the person?
What to expect from your doctor
Your healthcare professional is likely to ask you several questions, including:
- When did you first experience symptoms?
- Are your symptoms continuous or do they come and go?
- How severe are your symptoms?
- What, if anything, helps improve your symptoms?
- Does anything make your symptoms worse?
© 1998-2026 Mayo Foundation for Medical Education and Research(MFMER). All rights reserved. Terms of Use
