Medulloblastoma
Conditions
Overview
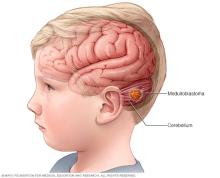
Medulloblastoma (muh-dul-o-blas-TOE-muh) is a cancerous, also called malignant, brain tumor that starts in the back and lower part of the brain.
This part of the brain is called the cerebellum. The cerebellum helps control balance, movement and coordination.
Medulloblastoma is the most common cancerous brain tumor in children, though it also can happen in adults.
Medulloblastoma forms when cells in the cerebellum develop changes in their DNA. These changes cause the cells to grow and multiply quickly. The tumor can press on nearby parts of the brain and may block the flow of cerebrospinal fluid. This can cause pressure to build up in the brain.
Medulloblastoma can spread, also known as metastasize, to other parts of the brain and spinal cord through cerebrospinal fluid. It rarely spreads outside the central nervous system.
There are four main types, also called molecular groups, of medulloblastoma. These groups are defined by the tumor’s genetic features. The four groups are WNT-activated, SHH-activated (including TP53-mutant and TP53-wildtype), group 3 and group 4.
Group 3 and group 4 tumors are sometimes described together as non-WNT and non-SHH tumors, although they are separate groups. Knowing the tumor type helps guide treatment.
Hearing this diagnosis can feel overwhelming. It may help to know that, with treatment, many children with medulloblastoma live well beyond five years after diagnosis.
Every child's situation is different. The outlook depends on several factors, including age, tumor type, whether the cancer has spread and how much of the tumor can be safely removed.
The type of medulloblastoma is based on how the tumor cells look under a microscope and on lab tests that look at changes in the tumor's genes. The type of medulloblastoma helps guide treatment and can affect survival.
All medulloblastomas are considered grade 4 tumors. The subtypes below describe the tumor's molecular features, not its grade.
Molecular types
Most medulloblastomas can be grouped into four main types based on changes in their genes. These tumor types include:
- WNT-activated (wingless/integrated). WNT is the name of a cell signaling pathway involved in brain development. WNT-activated tumors are one of the less common medulloblastoma types. They often respond very well to treatment and are linked to the best survival rates. They are most often seen in older children and teens.
- SHH-activated (sonic hedgehog). Sonic hedgehog is the name of a cell growth signaling pathway involved in brain development. SHH medulloblastoma can occur in infants, children and adults. Survival varies depending on other tumor features and gene changes. Some SHH tumors, known as SHH-activated TP53-wildtype, behave less aggressively. Other SHH tumors, called SHH-activated TP53-mutant, may be harder to treat.
- Group 3. Group 3 medulloblastoma is more common in young children. These tumors are non-SHH and non-WNT molecular types. It tends to grow and spread more quickly than other types. It may be harder to treat and is often linked to lower survival rates compared with WNT tumors.
- Group 4. Group 4 medulloblastoma is the most common type. These tumors are non-SHH and non-WNT molecular types. It can occur in children and adults. Its behavior varies. Some tumors respond well to treatment, while others may spread at diagnosis.
The numbering starts at 3 and 4 because the first two groups were named WNT-activated and SHH-activated based on specific gene patterns.
Cell appearance types
Medulloblastoma also can be described based on how the cells look under a microscope although genetic and molecular features are increasingly used for diagnosis and understanding outcomes. These include:
- Classic.
- Desmoplastic or nodular.
- Large cell or anaplastic.
These features also help healthcare professionals understand how the tumor may behave.
How is medulloblastoma different from other brain tumors?
Medulloblastoma is different from many other types of brain tumors. These tumors differ in where they start, who they affect and how they are treated.
Here's how they compare:
- Medulloblastoma versus glioma. Medulloblastoma is not a glioma. Gliomas form from support cells in the brain called glial cells. Medulloblastoma forms from developing nerve cells in the cerebellum.
- Medulloblastoma versus glioblastoma. Glioblastoma is an aggressive brain tumor that usually affects adults and starts in the upper parts of the brain. Medulloblastoma is more common in children and often responds better to treatment.
- Medulloblastoma versus ependymoma. Ependymomas begin in cells that line the fluid-filled spaces of the brain and spinal cord. Medulloblastoma tends to grow in the cerebellum and is more likely to spread through cerebrospinal fluid.
Symptoms

Symptoms of medulloblastoma happen when the tumor grows and presses on parts of the brain. The tumor also can block the usual flow of cerebrospinal fluid. This can cause pressure to build inside the head.
Common signs and symptoms of medulloblastoma may include:
- Dizziness.
- Double vision or other vision changes.
- Headaches, which are often worse in the morning.
- Nausea or vomiting.
- Poor coordination.
- Tiredness.
- Difficulty with balance or an unsteady walk.
Headaches and vomiting often happen because of the buildup of pressure inside the skull.
Symptoms in young children and infants
In young children, symptoms may develop over several weeks. Children may have trouble walking, seem clumsy or lose balance. Infants may have an increase in head size, unusual sleepiness or feeding difficulties.
Symptoms in children and adults
Symptoms of medulloblastoma are generally similar in adults and children because the tumor usually starts in the same part of the brain. Both may have headaches, balance difficulties and nausea.
Can you feel a medulloblastoma tumor?
Medulloblastoma grows deep inside the brain. It does not usually cause a lump or bump that you can feel on the outside of the head.
When to see a doctor
Make an appointment with your healthcare professional if you or your child has symptoms that worry you, especially ongoing headaches, repeated vomiting, or new issues with balance or vision.
Causes
It's not clear what causes medulloblastoma. This cancer starts as a growth of cells in the lower back part of the brain, called the cerebellum.
DNA contains instructions that tell cells how to grow and function. In healthy cells, DNA controls how fast cells grow and when they die. In cancer cells, DNA changes give different instructions. These changes tell cancer cells to grow and multiply quickly. Cancer cells can keep living when healthy cells would die. This leads to too many cells that form a tumor.
The tumor can grow and press on nearby brain structures. Medulloblastoma cells also can metastasize to other parts of the brain and spinal cord through cerebrospinal fluid.
Risk factors
Risk factors are things that may increase the chance of developing medulloblastoma. Most people with medulloblastoma do not have a known risk factor.
- Young age. These tumors can happen at any age, but they happen most often in children.
- Inherited syndromes. Most cases of medulloblastoma are not inherited. However, the tumor happens more often in people with certain rare genetic conditions that increase cancer risk. These include Fanconi anemia, Gorlin syndrome, Li-Fraumeni syndrome, Rubinstein-Taybi syndrome and Turcot syndrome.
There are no known lifestyle or environmental risk factors for medulloblastoma.
Diagnosis
Diagnosis usually begins with a physical exam, review of medical history and a discussion of symptoms.
Tests and procedures used to diagnose medulloblastoma include:
- Neurological exam. The exam tests vision, hearing, balance, coordination and reflexes. It can help show which part of the brain may be affected by the tumor.
- Imaging tests. Imaging tests take pictures of the brain. MRI is the main test used to diagnose medulloblastoma. A brain MRI can show the size and location of the tumor. It also can show increased pressure or a blockage in the flow of cerebrospinal fluid. MRI of the spine is often done to check whether the tumor has spread through cerebrospinal fluid. This helps determine the risk group of the cancer. Brain CT scans may be used in certain situations, including emergencies.
- Tissue sample testing. A tissue sample is usually taken during surgery to remove the tumor. This procedure is called a brain biopsy. A biopsy is a procedure to remove a sample of tissue for testing in a lab. The sample is tested in a lab to confirm that it is medulloblastoma. A separate biopsy alone is uncommon and is used only in certain situations.
- Removal of cerebrospinal fluid for testing. A lumbar puncture involves inserting a needle between two bones in the lower back. The needle removes cerebrospinal fluid from around the spinal cord. The fluid is tested in a lab to look for tumor cells. This test is done only after pressure in the brain is treated or after surgery.
Medulloblastoma is classified as a grade 4 tumor. In brain tumors, grade refers to how fast the tumor is likely to grow and how aggressive it may be if not treated. Grade 4 tumors tend to grow quickly and require prompt treatment. Doctors use imaging results, spinal fluid testing and lab testing of the tumor to determine the tumor's risk group and guide treatment.
Treatment
Treatment for medulloblastoma usually includes surgery followed by radiation therapy, chemotherapy or both. Many children can be treated successfully, especially when the tumor is found early and has not spread.
The exact treatment plan depends on several factors, including:
- How much of the tumor can be safely removed.
- Whether the tumor has spread to the brain or spinal cord.
- The results of lab tests on the tumor.
- The person's age and overall health.
Doctors use this information to decide how strong the treatment needs to be. Some tumors require more-intensive treatment, while others may be treated with lower doses to reduce long-term side effects.
Treatment options include:
- Surgery to relieve fluid buildup in the brain. A medulloblastoma may block the flow of cerebrospinal fluid. This can cause fluid to build up and increase pressure in the brain, which is called hydrocephalus. To reduce the pressure, a surgeon may create a new pathway for the fluid to drain safely. Sometimes this is done at the same time as tumor removal.
- Brain tumor surgery to remove the medulloblastoma. The goal is to remove as much of the tumor as safely possible. Sometimes the tumor cannot be fully removed because it is close to parts of the brain involved in walking, talking and other important functions. Most people need more treatment after surgery to destroy remaining cancer cells.
- Radiation therapy. Radiation therapy uses high-energy beams to kill cancer cells. Radiation is usually given to both the brain and spinal cord, followed by a focused boost to the area where the tumor started. Proton beam therapy may be used in some centers to reduce radiation to nearby healthy tissue. Radiation therapy is often given after surgery.
- Chemotherapy. Chemotherapy treats cancer with strong medicines. These medicines are usually given through a vein. Chemotherapy may be given after surgery, after radiation therapy or at the same time as radiation. In very young children, chemotherapy may be used to delay or avoid radiation therapy to protect the developing brain.
- Clinical trials. Clinical trials study new treatments or new ways to combine surgery, radiation and chemotherapy. Participation may provide access to newer therapies. Talk with your healthcare professional to learn if a clinical trial may be an option.
Treatment in children versus adults
Treatment for medulloblastoma is similar in children and adults, but there are important differences. Older children often receive radiation to the brain and spinal cord followed by chemotherapy. In very young children, doctors may delay or reduce radiation to protect the developing brain.
Adults also may receive surgery, radiation and chemotherapy. But treatment plans for adults may be adjusted based on age, overall health and side effects.
Preparing for an appointment
Make an appointment with a doctor or other healthcare professional if you have any symptoms that worry you.
Because appointments can be brief, it's a good idea to be prepared. Here's some information to help you get ready.
What you can do
- Be aware of anything you need to do ahead of time. At the time you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your diet.
- Write down symptoms you have, including any that may not seem related to the reason for which you scheduled the appointment.
- Write down important personal information, including major stresses or recent life changes.
- Make a list of all medicines, vitamins or supplements you're taking and the doses.
- Take a family member or friend along. Sometimes it can be very hard to remember all the information provided during an appointment. Someone who goes with you may remember something that you missed or forgot.
- Write down questions to ask your healthcare team.
Your time with your healthcare team is limited, so preparing a list of questions can help you make the most of your time together. List your questions from most important to least important in case time runs out. For medulloblastoma, some basic questions to ask include:
- Do I have a medulloblastoma?
- Will I need more tests?
- Can my medulloblastoma be removed?
- Why do I need additional treatments if surgery removes the entire medulloblastoma?
- What are the treatment options?
- What is the stage of my medulloblastoma?
- Has my medulloblastoma spread to other parts of my body?
- How much does each treatment increase my chances of a cure or prolong my life?
- What are the potential side effects of each treatment?
- How will each treatment affect my daily life?
- Is there one treatment option you believe is the best?
- What would you recommend to a friend or family member in my situation?
- Should I see a specialist?
- Are there any brochures or other printed material that I can take with me? What websites do you recommend?
- What will determine whether I should plan for a follow-up visit?
- Will I need to continue coming back?
Don't hesitate to ask other questions.
What to expect from your doctor
Be prepared to answer questions, such as:
- When did your symptoms begin?
- Have your symptoms been continuous or occasional?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Survival rates
Survival rate describes the percentage of people who are alive a certain number of years after diagnosis. Survival depends on age, whether the tumor has spread and the tumor's molecular type.
Survival in children
Factors such as age, tumor type, and whether or not the tumor has metastasized can affect survival rates.
-
Five-year survival. About 70% to 85% of children with average-risk medulloblastoma are alive five years after diagnosis. Average risk means the tumor has not spread and most of it was removed during surgery.
Many children with average-risk medulloblastoma can be cured with treatment.
Survival is lower when the tumor has spread to the brain or spinal cord at diagnosis or when a large amount of tumor remains after surgery. In these higher risk cases, five-year survival may be closer to 60%.
- 10-year survival. Long-term survival beyond five years is common, especially when the tumor has not spread and responds well to treatment.
Survival in children with medulloblastoma depends mainly on the type of tumor and whether it has metastasized.
- WNT-activated. Children with WNT-activated medulloblastoma often have the highest survival rates. With treatment, the five-year survival rate can be higher than 90%.
- SHH-activated. Survival varies in SHH-type tumors. Some respond well to treatment, especially when certain high-risk gene changes are not present, such as with SHH-activated TP53-wildtype. Other SHH tumors, such as SHH-activated TP53-mutant, may grow faster, metastasize more easily or be harder to treat.
- Group 3. Group 3 tumors tend to be more aggressive, especially when the tumor has metastasized. Survival rates are generally lower than in WNT-activated tumors.
- Group 4. This type is the most common type of medulloblastoma. Survival is usually between that of WNT-activated and group 3 tumors and depends on whether the tumor has metastasized and other features.
Infants and very young children may have lower survival rates because radiation treatment is limited to protect brain development.
Survival in adults
Survival rates in adults depend on the tumor type and whether the cancer has metastasized. Outcomes also are affected by how much tumor remains after surgery and by tumor features linked to faster growth. Survival may be lower in adults whose tumors have spread or have large cell features.
- Five-year survival rate. In a modern single-center study of adults treated with surgery, radiation therapy and chemotherapy, about 86% were alive five years after diagnosis.
- 10-year survival rate. Research shows that about 64% of adults were alive 10 years after diagnosis.
Recurrence rates
The cancer grows back, also called recurs, after treatment in about 20% to 30% of children with medulloblastoma. The risk of recurrence is higher when the tumor has metastasized by the time of diagnosis or in certain tumor types, such as some group 3 tumors.
Most recurrences in children happen within the first three years after diagnosis, often within the first year in those at higher risk. In adults, recurrence may occur later.
Recurrence can happen in the original tumor area, elsewhere in the brain or in the spinal cord. When medulloblastoma comes back, it is usually harder to treat and survival rates are lower.
Prognosis
Prognosis refers to the likely outcome of a disease. With treatment options available today, many children with medulloblastoma survive for many years after diagnosis. Outcomes vary based on several factors.
Adults and children may experience the disease differently. Children are more likely to have long-term side effects from treatment that affect growth, learning and hormone function. These effects can include slower physical development, difficulty with memory or attention, and changes in puberty or fertility. Adults may experience later recurrences and treatment-related side effects that affect work and daily activities.
What affects prognosis?
The outlook for medulloblastoma depends on:
- The person's age.
- Whether the tumor has metastasized to the brain or spinal cord.
- How much of the tumor was safely removed during surgery.
- The tumor's molecular type, such as WNT-activated, SHH-activated (TP53-wildtype or TP53-mutant), group 3 or group 4.
- Results of lab testing of the tumor cells.
Tumors that have not spread and can be mostly removed often have better outcomes. Some molecular types, such as WNT-activated tumors, are linked to higher survival rates. Others, such as certain group 3 tumors, may be more aggressive and have a poorer prognosis.
Is medulloblastoma curable?
Many children with medulloblastoma can be cured, especially when the tumor is found early and has not spread. Adults also can be successfully treated, but outcomes may vary more widely.
© 1998-2026 Mayo Foundation for Medical Education and Research(MFMER). All rights reserved. Terms of Use
