Fatty liver disease (MASLD)
Conditions
Overview
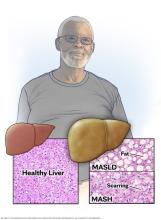
Metabolic dysfunction-associated steatotic liver disease (MASLD), formerly called nonalcoholic fatty liver disease (NAFLD), is a liver condition that affects people with excess weight, obesity or other metabolic conditions, such as type 2 diabetes, high blood pressure or high cholesterol. In MASLD, too much fat builds up in the liver.
MASLD is becoming more common, especially in Middle Eastern and Western nations, as the number of people with obesity rises. It is the most common form of liver disease in the world. MASLD ranges in severity from hepatic steatosis — sometimes called diffuse hepatic steatosis, or formerly fatty liver infiltration or simply fatty liver — to a more severe form of disease called metabolic dysfunction-associated steatohepatitis (MASH), formerly called nonalcoholic steatohepatitis (NASH).
MASH causes the liver to swell or enlarge. This is known as hepatomegaly. MASH also causes fat deposits in the liver, which causes liver damage. MASH may get worse and may lead to serious liver scarring, called cirrhosis, or even liver cancer. This damage is like the damage caused by heavy alcohol use.
Life expectancy varies depending on whether you have MASLD or MASH. Factors such as scarring and other health conditions also affect how long you can live with MASLD or MASH.
Symptoms
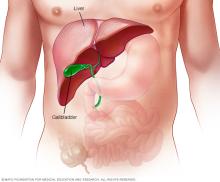
MASLD often has no symptoms. When it does, they include:
- Feeling very tired, also called fatigue.
- Not feeling well, known as malaise.
- Pain or discomfort in the upper right belly area.
Possible symptoms of MASH and cirrhosis, which is severe scarring, include:
- Itchy skin.
- Abdominal swelling, also called ascites (uh-SY-teez).
- Shortness of breath.
- Swelling in the legs.
- Spiderlike blood vessels just beneath the skin's surface.
- Enlarged spleen.
- A change in skin color on the palms.
- Yellowing of the skin and eyes, also called jaundice.
When to see a doctor
Make an appointment with a member of your health care team if you have lasting symptoms that worry you.
Causes
Experts don't know exactly why fat builds up in some livers and not others. They also don't fully understand why fat buildup in some livers turns into MASH.
MASLD and MASH are both linked to the following:
- Genetics.
- Being overweight or having obesity.
- Insulin resistance, which happens when the body's cells don't take up sugar in response to the hormone insulin.
- Type 2 diabetes, sometimes called high blood sugar or hyperglycemia.
- High levels of fats, especially triglycerides, in the blood.
These combined health concerns may contribute to liver damage. However, some people get MASLD even if they do not have any risk factors.
Risk factors
Many diseases and health conditions can increase your risk of MASLD, including:
- Obesity, especially when fat is centered in the waist.
- Type 2 diabetes.
- High cholesterol.
- High levels of triglycerides in the blood.
- Insulin resistance.
- Metabolic syndrome.
- Polycystic ovary syndrome.
- Obstructive sleep apnea.
- Underactive thyroid, also called hypothyroidism.
- Underactive pituitary gland, also called hypopituitarism.
- Growth hormone deficiency, which means the body doesn't make enough hormones to grow.
MASH is more likely in people:
- Older than 50.
- Who have certain genetic risk factors.
- With obesity.
- With diabetes or high blood sugar.
- With symptoms of metabolic syndrome, such as high blood pressure, high triglycerides and a large waist size.
It is hard to tell MASLD and MASH apart without an exam and testing.
Complications
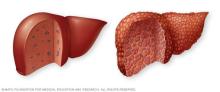
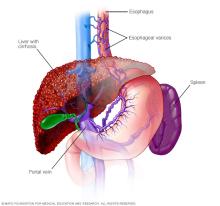
Severe liver scarring, also called cirrhosis, is the main complication of MASLD and MASH. Cirrhosis happens because of liver injury, such as the damage caused by inflammation in MASH. As the liver tries to stop inflammation, it creates areas of scarring, also called fibrosis. With ongoing inflammation, fibrosis spreads and takes up more liver tissue.
If nothing is done to stop the scarring, cirrhosis can lead to:
- Fluid buildup in the stomach area, called ascites.
- Swollen veins in the esophagus, called esophageal varices, which can rupture and bleed.
- Confusion, sleepiness and slurred speech, also called hepatic encephalopathy.
- Overactive spleen, known as hypersplenism, which can cause too few blood platelets.
- Liver cancer.
- End-stage liver failure, which means the liver has stopped working.
For many people with MASLD, the outlook is good, especially if they make recommended lifestyle changes. In fact, in some people, weight loss may help reverse MASLD. However, some people develop MASH, which significantly impacts life expectancy and health outcomes.
Prevention
To reduce your risk of MASLD:
- Eat a healthy diet. Eat a diet that's rich in fruits, vegetables, whole grains and healthy fats. One such diet is the Mediterranean diet.
- Limit alcohol, simple sugars and portion sizes. Avoid sugary drinks such as soda, sports drinks, juices and sweet tea. Avoid or limit alcohol, which can damage the liver.
- Keep a healthy weight. If you are overweight or have obesity, work with your healthcare team to gradually lose weight. If you are at a healthy weight, work to keep it by eating a healthy diet and exercising.
- Exercise. Be active most days of the week. Get an OK from your healthcare team first if you haven't been exercising regularly.
Diagnosis
Because MASLD typically causes no symptoms, it is often found when tests done for other reasons point to a liver condition. For example, a blood test done during a yearly exam may show high levels of liver enzymes, which can prompt more testing that leads to a MASLD diagnosis.
Tests done to diagnose MASLD, rule out other diseases and see how bad the liver damage is include:
Blood tests
- Liver enzyme and liver function tests.
- Complete blood count.
- Iron studies, which show how much iron is in the blood and other cells.
- Tests for chronic viral hepatitis, which includes hepatitis B and hepatitis C.
- Celiac disease screening test.
- Measurement of fasting blood sugar.
- A1C test, which shows how stable your blood sugar is.
- Lipid profile, which measures blood fats such as cholesterol and triglycerides.
Imaging procedures
Imaging tests used to diagnose MASLD include:
- Abdominal ultrasound, which is often the first test used when liver disease is suspected.
- Magnetic resonance imaging (MRI) or computerized tomography (CT) scanning. These tests are better at finding excess liver fat and cirrhosis.
- Transient elastography, a newer type of ultrasound that measures the stiffness of the liver. Liver stiffness is a sign of scarring, also called fibrosis.
- Magnetic resonance elastography, which combines MRI with sound waves to create a visual map, also called an elastogram, showing the stiffness of body tissues.
Liver biopsy
If other tests show signs of MASH, or if your test results are unclear, your healthcare professional may suggest a liver biopsy. Liver biopsy is a procedure to remove a small piece of tissue from your liver. It is usually done using a needle passed through the abdominal wall. The tissue sample is looked at in a lab for signs of inflammation and scarring. Liver biopsy is a way to diagnose MASH and find out the amount of liver damage, but in most people, noninvasive imaging tests are used instead.
You may feel some discomfort with a liver biopsy, and it does have risks that your healthcare team talks about with you in detail.
Treatment
Treatment for MASLD usually starts with weight loss. This can be done by eating a healthy diet, limiting portion sizes and exercising. Losing weight may improve other health conditions that can lead to MASLD. Typically, losing 10% of your body weight or more is recommended. But losing even 3% to 5% of your starting weight can have benefits.
Two medicines are available to treat people who have MASH with moderate to severe liver scarring. Resmetirom (Rezdiffra) and semaglutide can help reduce the amount of fat and scarring in the liver. These medicines are not recommended for people with cirrhosis. People who have cirrhosis due to MASH may need a liver transplant.
With help from your health care team, you can take steps to manage nonalcoholic fatty liver disease. You can:
- Lose weight. If you're overweight or obese, reduce the number of calories you eat each day and increase your physical activity to lose weight slowly. Eating fewer calories is key to losing weight and managing this disease. If you tried to lose weight in the past and couldn't, ask your health care team for help.
- Choose a healthy diet. Eat a healthy diet that's rich in fruits, vegetables and whole grains. Your health care team may suggest avoiding or limiting certain foods and drinks, such as white bread, red and processed meats, juices, and sweetened drinks. Keep track of all calories you take in.
- Exercise and be more active. Aim for at least 150 minutes of exercise a week. If you're trying to lose weight, you might find that more exercise is helpful. But if you don't already exercise regularly, get your health care team's OK first and start slowly.
- Manage your diabetes. Follow your health care team's advice to manage your diabetes. Take your medicines as told by your care team and watch your blood sugar closely.
- Lower your cholesterol and blood pressure. Improve your cholesterol levels and blood pressure if they are high. A healthy diet, exercise and medicines can help keep your cholesterol, triglycerides and blood pressure at healthy levels.
- Protect your liver. Avoid things that could harm your liver health. For example, don't drink alcohol. Follow the instructions on all medicines and nonprescription drugs. Check with your health care team before using any herbal supplements, as some can harm the liver.
Alternative medicine
No alternative medicine treatments are proved to cure MASH or MASLD. But researchers are studying whether some supplements or natural compounds could be helpful, such as:
-
Vitamin E. In theory, vitamin E and other vitamins called antioxidants could help protect the liver by lessening or canceling out the damage caused by inflammation. But more research is needed.
Some evidence suggests that vitamin E supplements may be helpful for people with MASLD who don't have type 2 diabetes. Vitamin E supplements are not recommended for people with serious liver scarring or type 2 diabetes. Vitamin E has been linked with a slightly increased risk of heart disease and prostate cancer.
- Caffeinated coffee. Some studies suggest that coffee may benefit the liver by reducing the risk of liver diseases such as MASLD and lowering the chance of scarring. It's not yet clear how coffee may prevent liver damage. But certain compounds in coffee are thought to lower inflammation and slow scar tissue growth.
If you already drink coffee, these results may make you feel better about your morning cup. But if you don't already drink coffee, this probably isn't a good reason to start. Discuss the possible benefits of coffee with your healthcare team.
Preparing for an appointment
See your family or primary healthcare professional first if you have symptoms that worry you. If a liver problem such as MASLD or MASH is suspected, you may be referred to a doctor who specializes in the liver, called a hepatologist.
Because appointments can be short, it's a good idea to be well prepared. Here are a few tips to help you get ready, and what to expect from your healthcare professional.
What you can do
- Know what to do before your visit. When you make the appointment, ask if there's anything you need to do beforehand.
- Write down any symptoms you're having. Include any that may not seem related to the appointment.
- Make a list of all medications, vitamins and supplements you're taking.
- Take any relevant medical records. Examples include the results of any tests you've had that relate to your current condition.
- Take a family member or friend along, if possible. Sometimes it can be hard to remember all the information you get during an appointment. Someone who comes with you may remember something that you missed or forgot.
- Write down questions to ask your healthcare team.
If you find out you have MASH or MASLD, some basic questions to ask include:
- Is the fat in my liver hurting my health?
- Will my condition disease become serious?
- What are my treatment options?
- What can I do to keep my liver healthy?
- I have other health issues. How can I best manage them together?
- Should I see a specialist? Will my insurance cover it?
- Are there any brochures or other printed material that I can take with me? What websites do you recommend?
- Should I plan for a follow-up visit?
In addition to the questions that you've prepared to ask your care team, don't hesitate to ask questions during your appointment.
What to expect from your doctor
Your healthcare professional is likely to ask you a number of questions, such as:
- Have you had any symptoms, such as yellowing of the eyes or skin and pain or swelling around your waist?
- If you've had tests done for these symptoms, what were the results?
- Do you drink alcohol?
- What medicines do you take, including medicines you buy without a prescription and supplements?
- Have you ever been told that you have hepatitis?
- Do other people in your family have liver disease?
Stages
Fibrosis staging is the most important factor in determining survival rates and prognosis. These stages are:
- F0: No scarring.
- F1: Mild scarring.
- F2: Moderate scarring.
- F3: Advanced scarring.
- F4: Cirrhosis.
The higher the stage, the more serious the condition.
Survival rates
Metabolic dysfunction-associated steatotic liver disease (MASLD) and metabolic dysfunction-associated steatohepatitis (MASH) are liver conditions that are becoming more common, especially in people with obesity, diabetes, high blood pressure and high cholesterol. These diseases used to be called nonalcoholic fatty liver disease (NAFLD) and nonalcoholic steatohepatitis (NASH), but experts updated the names to better reflect their connection to metabolic health.
MASLD means your liver has too much fat. This can happen even if you don't drink alcohol. MASLD is often found in people who are overweight or have diabetes. More than one-third of the world's population has MASLD.
MASH is a more serious form of liver disease. It means your liver is not only fatty but also inflamed and damaged.
Which of these liver conditions you have, along with several other factors, is key to understanding your outlook, also called prognosis.
© 1998-2026 Mayo Foundation for Medical Education and Research(MFMER). All rights reserved. Terms of Use
