Periprosthetic joint infection (PJI)
Conditions
Overview
A periprosthetic joint infection (PJI) happens when bacteria or other microorganisms infect the area in and around a joint implant. This could include infection around a hip, knee, shoulder or elbow replacement. In medical terms, "peri" means around or surrounding.
This kind of infection can happen soon after joint replacement surgery. Or it can happen months or even years later. Some infections are long-lasting. These are called chronic. Others come on more suddenly. These are called acute.
PJI is treatable but often needs a combination of antibiotics and surgery.
Symptoms
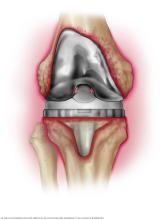
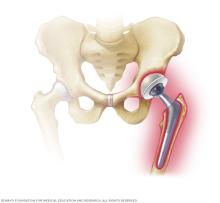
Recognizing symptoms of a periprosthetic joint infection (PJI) early is important. It is a serious condition that needs treatment right away. Common symptoms of PJI include:
- Drainage or fluid coming from the incision site.
- Increasing pain.
- Swelling that gets worse around the joint.
- A change in skin color or warmth around the joint.
- Fever and chills.
When to see a doctor
Call your surgeon or seek medical care right away if you have had a joint replacement and notice these signs of a serious infection:
- Fever plus joint pain, swelling and warmth.
- Confusion.
- Sudden trouble walking or bearing weight.
- A change in skin color around the joint that spreads or grows.
Causes
Periprosthetic joint infections (PJI) can be caused by:
- Microorganisms that get into your body after your joint replacement surgery. This happens before the surgical wound has completely healed.
- An infection nearby in the body that spreads to the joint.
- Bacteria carried in the bloodstream to the joint from another infection in your body.
The immune system typically fights off microorganisms such as bacteria or fungi when they enter your body. But the immune system can have a harder time when microorganisms stick to metal and plastic parts in your joint implant. These parts do not get blood flow. That means your immune system cannot easily find and fight the bacteria. Many microorganisms can form a coating called a biofilm. It helps them hide from the immune system and antibiotics.
Often, it is hard to know exactly how the infection began.
Risk factors
Some people are at higher risk of developing a periprosthetic joint infection (PJI) after joint replacement. These risk factors make it hard to fight an infection:
- Diabetes.
- Poor circulation.
- Obesity.
- Smoking.
- A weakened immune system from conditions such as cancer.
- Treatments that lower the immune system, such as chemotherapy or corticosteroids.
Prevention
Periprosthetic joint infection (PJI) is uncommon, but you and your healthcare team can take steps to help prevent PJI.
Before joint replacement surgery, try to be as healthy as possible. This may include managing blood sugar if you have diabetes and stopping smoking. Your healthcare team may check for any active infections and treat them before surgery.
During and after surgery, your healthcare team uses strict sterile techniques and may give antibiotics before, during and after the operation to prevent infection.
After surgery, good wound care is important. Watch for warning signs such as increasing pain, fever, swelling, a change in skin color, or drainage from the incision. Treating infections elsewhere in the body quickly also helps protect the new joint. While PJI cannot always be prevented, these steps can lower the risk.
Diagnosis
To diagnose a periprosthetic joint infection (PJI), your healthcare team may use a combination of a physical exam, lab tests, imaging tests and joint fluid tests. Your care team may include experts from orthopedic surgery and infectious disease.
Lab tests
Typically, to diagnose PJI, your healthcare team will order the following blood tests to look for signs of infection or swelling and irritation, also called inflammation:
- Complete blood count (CBC).
- C-reactive protein (CRP).
- Erythrocyte sedimentation rate (ESR).
Other lab tests may be needed. The healthcare professional often takes a sample of joint fluid using a needle. This is called a joint aspiration. The fluid samples are sent to the lab to check for signs of infection and perform cultures.
For cultures, the joint fluid is kept warm, like your body temperature, so any microorganisms in the fluid can grow.
Over days or weeks, microbiologists and infectious disease experts watch to see what kind of microorganisms grow. Most periprosthetic joint infections are caused by bacteria rather than fungi. Knowing what causes your infection helps your care team choose the right antibiotics to treat the infection.
Imaging tests
Imaging tests help your care team see if your implant is loose. The tests also may show if there is an infection in or around your joint. Imaging tests may include:
- X-rays. These are usually the first imaging tests done. They can show changes around the implant or if the implant has come loose.
- MRI or CT scans. These scans can show more-detailed images of soft tissues and can show fluid around the joint.
- Bone scans. These images help to show areas of increased bone activity, which can be caused by infection.
Identifying infection type: Acute vs. chronic
Treatment options that may be right for you depend on the type of periprosthetic joint infection (PJI) you have. As part of your diagnosis, your healthcare team figures out if you have an acute or a chronic infection. Acute means it has started more recently. Chronic means the infection is long-lasting.
- Acute PJI. This typically happens within about six weeks of joint replacement surgery. Or it can happen suddenly in a prosthetic joint that has been working well. Symptoms can come on quickly. These infections usually start when microorganisms get into the new joint during surgery, while the surgical cut is healing or from your bloodstream.
- Chronic PJI. This typically develops more than three months after your joint replacement surgery. Sometimes the cause of the infection is not known. Symptoms may progress slowly, over months or even years.
Treatment
If you have an infected artificial joint and the periprosthetic joint infection (PJI) is caught early, you don't always have to have the joint removed. But you likely need surgery. If you have had the infection for several weeks or months, you typically must have the artificial joint removed.
How your infected joint is treated depends on how long you have had the infection. It also depends on:
- The cause of your infection.
- The condition of your joint replacement.
- The health of your soft tissues and bone.
- Your other medical conditions.
Most treatment plans involve both antibiotics and surgery. It is common to need more than one surgery to treat periprosthetic joint infection. You may need to take antibiotics for several weeks or even months before and after any surgery.
Antibiotics
Antibiotic therapy is a part of treatment before and after surgeries for PJI. Usually, therapy starts with IV antibiotics and then sometimes changes to oral antibiotics. How long antibiotic therapy lasts depends on the treatment approach. Sometimes you need antibiotics for weeks, months or even longer.
For people who can't have major surgery or who have an ongoing infection risk, long-term oral antibiotics may be used to control, but not cure, the infection.
Surgery
Most PJIs are treated with surgery. Common approaches include:
- Debridement, antibiotics and implant retention (DAIR). During this procedure, the surgeon cleans out the joint and removes any infected tissue. The goal is to clear the infection while keeping the implant in place. The surgeon may replace plastic liners or parts. After surgery, your healthcare team prescribes IV or oral antibiotics. DAIR is most often used for acute infections.
- One-stage revision. During this procedure, the surgeon removes the infected artificial joint and cleans out the joint area. The surgeon puts in a new, clean implant during this same surgery. Antibiotic cement may be used to fix the new joint. This special medical cement has antibiotic medicine that helps fight infection. You are given IV or oral antibiotics to take for several months after surgery. This surgery is recommended only when the bacteria causing the infection is known before surgery and the bone and tissue around the joint are healthy.
-
Two-stage revision. This is the most common approach for chronic and complex infections. It involves two surgeries. In the first surgery, the surgeon removes the infected implant and cleans out the joint area. The surgeon then puts an antibiotic spacer in the joint. The spacer is a temporary part placed in the joint while the infection heals. It is fixed to the bone with cement that has antibiotic medicine that kills bacteria.
The spacer helps keep the joint in place until a new implant is put in. The surgeon may perform flap surgery if needed. Flap surgery helps the wound heal. It uses healthy tissue such as skin, fat or muscle that has its own blood supply. The surgeon moves the tissue to cover the wound and bring blood flow to the area. More blood flow helps the wound heal. It lowers the chance of another infection. You are given IV or oral antibiotics for six or more weeks between surgeries. Your care team monitors you for a time after surgery, when you are not on antibiotics. This is done to make sure that the infection is gone.
Then a second surgery removes the spacer, cleans out the joint again, and implants a new, clean total joint. The surgeon may adjust or reuse the earlier flap to make sure strong, healthy tissue covers the joint. You may need more antibiotics after the second surgery.
- Permanent joint removal, called resection arthroplasty. During this procedure, the surgeon cleans out the infection, removes the joint and does not replace it. Removing the joint may lessen pain, but the leg will not move or work like a healthy joint. You're given IV or oral antibiotics for at least six weeks after surgery. You have permanent joint removal when the infection can't be controlled. Or you may have it if you're not a good candidate for another joint replacement.
- Joint fusion, called arthrodesis. Joint fusion surgery permanently joins the bones. This can treat the infection and make the joint more stable. But you lose motion in the joint, and the limb may be shorter than before. You have IV or oral antibiotics for several weeks after surgery. This approach is used when a joint replacement is not a good option.
- Amputation. A surgeon may need to use limb amputation to treat life-threatening infections. Amputation is surgical removal of a body part, such as a toe, foot, arm or leg. Amputation also may be the best option if the bone and soft tissue surrounding the joint aren't healthy. The surgeon also may do surgery to amputate the limb when no other surgery can manage the infection. If any infected bone or tissue is left, you're given IV or oral antibiotics for several weeks after surgery.
Nonsurgical management of PJI
In rare cases, you may not have surgery for PJI. This usually happens if you already had several surgeries for infection or joint replacement and are still able to move around with little pain. In these situations, your healthcare professional may give you long-term oral antibiotics to take as long as the joint implant stays in place. The antibiotics help keep the infection under control. Antibiotics also stop the bacteria from causing increased symptoms around the joint or causing infections in other areas of the body.
This approach is not common. Most prosthetic hip or knee joint infections are treated with surgery, and often more than one surgery is needed to treat PJI. If your healthcare professional decides that surgery is not the right way to treat your infection, talk with your care team about what to expect.
Coping and support
Treatment for periprosthetic joint infection (PJI) is a long process. Over time, it can involve more than one surgery. You may start with one surgical treatment option but later may need another. It is important to know that PJI treatment may take months or even years. You can expect to have several appointments and may need many surgeries.
Having support helps you prepare for treatment. It also helps you recover afterward. Your caregiver can be a partner or spouse, a sibling, your adult child, or a close friend. Or you may have more than one caregiver over time. Being a caregiver takes time and energy. Make sure caregivers understand their commitment.
Your caregiver should come with you to your appointments and take part in the education about your treatment. The caregiver should be there when you have surgery and plan to support you with recovery and physical therapy after surgery.
Preparing for an appointment
During periprosthetic joint infection (PJI) treatment, your healthcare team may include experts in orthopedic surgery, infectious disease, physical therapy, occupational therapy and more.
What you can do
As you prepare for your appointment, make a list of:
- Your symptoms and when they began.
- Medical conditions you have.
- All medicines, vitamins and other supplements you take, including doses.
- Questions to ask your healthcare team.
Take a family member or friend along, if possible, to help you remember everything you talk about with your care team.
What to expect from your doctor
Your healthcare professional is likely to ask you questions such as:
- When did your symptoms start?
- Have your symptoms been ongoing or on-and-off?
- How bad are your symptoms?
- Does anything seem to make you feel better?
- What things seem to make your symptoms worse?
© 1998-2026 Mayo Foundation for Medical Education and Research(MFMER). All rights reserved. Terms of Use
