Primary biliary cholangitis (PBC)
Conditions
Overview
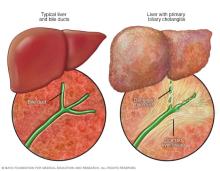
Primary biliary cholangitis (PBC) is an uncommon, long-term disease of the liver in which the body's immune system mistakenly attacks bile ducts within the liver. This gradually decreases the flow of bile from the liver to the small intestine. A buildup of bile damages and destroys liver tissues.
Primary biliary (BIL-ee-air-ee) cholangitis (koh-lan-JIE-tis) destroys the lining of the small- and medium-sized bile ducts that transport the digestive fluid bile from the liver. Leaking bile and related disease activity damage liver tissues. If left untreated, PBC can lead to scarring of tissues in the liver and liver failure. PBC most often affects middle-aged and older women.
Treatments for PBC include medicines to delay progression of the disease and to treat symptoms such as itching, extreme tiredness, and dry eyes and mouth. Advanced disease may require a liver transplant.
PBC was formerly called primary biliary cirrhosis.
Symptoms
More than 50% of people with primary biliary cholangitis do not have symptoms when they get a diagnosis. But symptoms appear at some point as damage to the liver worsens.
Symptoms often include:
- Fatigue.
- Itchy skin.
- Dry eyes and mouth.
- Difficulty with memory and concentration.
Other signs and symptoms may include:
- Pain in the upper right belly.
- Fatty deposits, called xanthomas, on the skin around the eyes or the creases of joints.
- Yellowing of the whites of the eyes or skin, called jaundice.
- Darkening of the skin that's not related to sun exposure.
- Oily or greasy stools.
When to see a doctor
Make an appointment with your healthcare professional if you have severe, persistent itching on much of your body with no obvious cause. Also, see your health professional if you feel extremely tired all the time, no matter how much rest you get.
Causes
Primary biliary cholangitis (PBC) is an autoimmune disease. This means the body's immune system attacks its own tissues as if it were fighting a disease.
Usually, certain types of white blood cells, called lymphocytes, find and attack germs or other foreign substances. In PBC, lymphocytes mistakenly target healthy cells lining the small- and medium-sized bile ducts in the liver. The immune system also makes disease-fighting proteins, called antibodies, that attack these healthy cells.
Bile ducts in the liver are gradually damaged and destroyed, causing bile to build up in the liver. This buildup is called cholestasis.
Leaking bile, inflammation and other immune system activity causes damage and scarring of liver tissues. This scarring, called fibrosis, leads to poor liver function. Eventually, fibrosis can lead to severe, permanent scarring, called cirrhosis.
It's not clear what triggers this autoimmune disease. Research suggests several potential triggers that may lead to PBC in people with a genetic risk of the disease. These triggers may include:
- Infections of the urinary tract or digestive tract.
- Cigarette smoking.
- Chemicals, including chemicals in some cosmetics.
- Environmental pollution.
Coexisting conditions
People with PBC often have another autoimmune disease. These may include:
- Thyroid disease.
- Rheumatoid arthritis.
- Sjogren syndrome, which causes dry eyes and mouth.
- Inflammatory bowel disease.
Risk factors
The following factors may increase your risk of primary biliary cholangitis:
- Sex assigned at birth. Most people with the disease are women.
- Age. It most often affects middle-aged and older adults.
- Genetics. You're more likely to get the condition if you have a family member who has or had it.
- Geography. It's most common among people in North America and Northern Europe.
Complications
As liver damage worsens, primary biliary cholangitis (PBC) can cause serious health problems, including:
- Liver scarring. Permanent liver scarring, also called cirrhosis, makes it difficult for your liver to work and may lead to liver failure. It occurs in later stages of primary biliary cholangitis.
- Portal hypertension. The portal vein is the major route for blood flowing into the liver. High blood pressure in this vein is called portal hypertension. This complication can cause pressure on blood vessels throughout the digestive system that can lead to life-threatening internal bleeding. Portal hypertension can cause enlargement of the liver and spleen and cause these organs to leak.
- Liver cancer. PBC increases the risk of liver cancer, particularly in people with cirrhosis of the liver.
- Thinning bones. People with PBC may experience thinning and weakened bones. This is called osteoporosis. Bones are brittle and can break easily.
- Vitamin deficiencies. Bile helps the intestines absorb vitamins A, D, E and K. PBC may result if the body does not get enough of these vitamins. This condition is called vitamin deficiency.
- High cholesterol. Up to 80% of people with PBC have high cholesterol.
Diagnosis
Your healthcare professional performs a physical exam and asks you about your health history.
The following tests and procedures are the primary means for making a diagnosis of primary biliary cholangitis (PBC).
- Liver function blood tests. Lab tests to check levels of certain proteins in the blood give your healthcare professional information about how well your liver is working. Certain results show a reduction in the transport of bile from the liver.
- Antibody tests. Most people with PBC have a positive test for immune system antibodies targeting cells of the lining of the bile ducts. This is called an antimitochondrial antibody (AMA) test.
- Liver biopsy. With a liver biopsy, a needle is used to remove a piece of liver that can be studied in a lab. An exam of the biopsy under a microscope can show the condition of the bile ducts and liver tissues. The test is usually used only if PBC is suspected, but antibody tests are negative.
Imaging tests
Imaging tests are usually not necessary to make a diagnosis. But they may be used to rule out other diseases or understand the condition of the liver. Imaging tests include:
- Ultrasound. Ultrasound images can show signs of other liver diseases such as tumors or blockages of bile ducts.
- Magnetic resonance imaging (MRI). MRI scans of the liver, bile ducts, gallbladder and pancreas can be used to rule out other diseases with similar signs and symptoms. The test is called a magnetic resonance cholangiopancreatography (koh-lan-jee-o-pan-cree-uh-TOG-ruh-fee).
- Elastography. These tests measure stiffness in liver tissue. The degree of stiffness indicates the degree of liver cirrhosis. Elastography may be done with an ultrasound, called a transient elastography. MRI-like tests, called magnetic resonance elastography (MRE), also can measure the degree of cirrhosis. Your healthcare team may use these tests to monitor disease progression.
Other tests
A test for cholesterol levels in the blood is common because cholesterol is often high in people with PBC.
Treatment
Treating the disease
Medicines may slow the progression of the primary biliary cholangitis (PBC) and prevent complications. Options include:
- Ursodiol (Actigall, Urso 250, Urso Forte) is the first line of treatment for PBC. Ursodiol is a naturally occurring bile acid that seems less likely to damage bile ducts than some other bile acids. By taking the place of more harmful bile acids, Ursodiol may result in improved liver function tests and delays in liver tissue damage. Ursodiol may reduce itching. Ursodiol is also called ursodeoxycholic acid,
- Fenofibrate (Lipofen) is approved for lowering cholesterol and triglycerides and increasing good cholesterol. It appears to have some benefit for improving liver function for people with PBC. It also may reduce itching and extreme tiredness.
- PPAR agonists affect mechanisms that regulate triglycerides and sugars in the body. These medicines are approved for treatment of PBC and can be taken with ursodiol. PPAR agonists, including elafibranor (Iqirvo) and seladelpar lysine (Livdelzi), may improve liver function.
Liver transplant
A liver transplant is the only treatment known to cure PBC. During a liver transplant, surgeons remove a diseased liver and replace it with a healthy liver from a donor.
A liver transplant is reserved for people with liver failure or other severe complications of PBC. The disease may appear again after a liver transplant.
Treating the symptoms
Your healthcare professional may recommend treatments to control the signs and symptoms of PBC and make you more comfortable.
Treatment for itching
- Antihistamines. Allergy medicines called antihistamines may help reduce mild itching. Because antihistamines can cause drowsiness, they may be good for people kept awake by itchiness.
- Bile acid sequestrants. Some medicines that bind to bile acids — the substances thought to cause itching in liver disease — are used to treat moderate to severe itching. These include cholestyramine (Locholest, Prevalite) and colestipol (Colestid). These medicines often cause constipation, cannot be used with several other medicine and may cause a vitamin K deficiency.
- Rifampin. Rifampin (Rifadin, Rimactane) is an antibiotic that may reduce moderate to severe itching. It may be used when bile acid sequestrants can't be used. Rifampin can cause liver inflammation, so blood tests are done regularly to test for side effects.
- Opioid antagonists. Naltrexone is an opioid antagonist that may reduce moderate to severe itching. This medicine is typically used for treating alcohol and opioid use disorders. Naltrexone can't be used if there is advanced liver disease.
Treatment for dry eyes and mouth
Artificial tears and saliva substitutes can help ease dry eyes and mouth. These are available with or without a prescription. You can make more saliva and relieve dry mouth by chewing sugarless gum, sucking on sugarless hard candy or eating dried fruit slices.
Treating the complications
Certain complications are commonly linked to PBC. Your healthcare professional may recommend:
- Vitamin and mineral supplements. If your body isn't absorbing vitamins or other nutrients, you may need to take vitamins A, D, E and K, as well as calcium, folic acid or iron supplements.
- Medicines to lower cholesterol. If you have high cholesterol levels in your blood, your healthcare professional may prescribe a medicine known as a statin.
- Medicines to treat bone loss. If you have weak or thinning bones, you may be prescribed medicines or supplements, such as calcium and vitamin D, to reduce bone loss and improve bone density. Exercise such as walking and using light weights most days of the week can help increase your bone density.
- Treatment for portal hypertension. Your healthcare professional is likely to screen and monitor you for portal hypertension and enlarged veins if you have more-advanced scarring from liver disease. Fluid may accumulate in the cavity that holds your digestive organs. For mild fluid accumulation, your healthcare professional may recommend limiting salt in your diet. More-severe cases may require medicines known as diuretics or a procedure to drain the fluid.
Lifestyle and home remedies
You may feel better if you take good care of your overall health. Here are some things you can do to improve some primary biliary cholangitis (PBC) symptoms and help prevent certain complications:
- Choose low-sodium foods. Eat low-sodium foods or naturally sodium-free foods. Sodium contributes to tissue swelling and the buildup of fluids.
- Avoid raw or undercooked food. Raw or undercooked seafood and meats and unpasteurized dairy products can carry bacteria. Bacterial infections can be dangerous for people with liver disease.
- Exercise most days of the week. Exercise may reduce your risk of bone loss.
- Avoid alcohol. Your liver processes the alcohol you drink, and the added stress can cause liver damage. Generally, people with primary biliary cholangitis should not drink alcohol.
- Check with your healthcare professional about medicines or dietary supplements. Because your liver isn't working well, you'll likely be more sensitive to the effects of over-the-counter and prescription medicines, as well as some dietary supplements. Check with your healthcare professional before taking anything new.
Coping and support
Living with liver disease with no cure can be frustrating. Fatigue alone can have a profound impact on your quality of life. Each person finds ways to cope with the stress of a long-term disease. In time, you'll find what works for you. Here are some ways to get started:
- Learn about your condition. The more you understand about primary biliary cholangitis (PBC), the more active you can be in your own care. In addition to talking with your healthcare professional, look for information at your local library and on websites affiliated with reputable organizations such as the American Liver Foundation.
- Take time for yourself. Eating well, exercising and getting enough rest can help you feel better. Try to plan ahead for times when you may need more rest.
- Get help. If friends or family want to help, let them. PBC can be exhausting, so accept the help if someone wants to do your grocery shopping, wash a load of laundry or cook your dinner. Tell those who offer to help what you need.
- Seek support. Strong relationships can help you maintain a positive attitude. If friends and family have a hard time understanding your illness, you may find that a support group can be helpful.
Preparing for an appointment
If you have signs or symptoms that worry you, make an appointment with your healthcare professional. If you're diagnosed with primary biliary cholangitis, you may be referred to a specialist in diseases of the digestive system, called a gastroenterologist, or a specialist in liver diseases, called a hepatologist.
Because there's often a lot to cover during your appointment, it's a good idea to arrive well prepared.
What you can do
- Be aware of any pre-appointment restrictions. At the time you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your diet.
- Write down any symptoms you're experiencing, including those that may seem unrelated to the reason for which you scheduled the appointment.
- Write down key personal information, including any major stresses or recent life changes.
- Make a list of all medicines, vitamins and supplements that you're taking, the doses and the reason for taking each one.
- Ask a family member or friend to come with you. Sometimes it can be difficult to remember all of the information provided to you during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your healthcare professional.
Preparing a list of questions can help you make the most of your time with your healthcare professional. Questions you may ask at your first appointment or follow-up care appointments may include:
- What kinds of tests do I need? Do these tests require any special preparation?
- How severe is the damage to my liver?
- How will we monitor the health of my liver?
- What treatments do you recommend for me?
- How will we know if I need a liver transplant?
- What types of side effects can I expect from treatment?
- Are there any other treatment options?
- What changes should I make to my diet?
- Are there brochures or other printed material that I can take with me? What websites do you recommend?
In addition to the questions that you've prepared to ask your healthcare professional, don't hesitate to ask other questions that come to mind during your appointment.
What to expect from your doctor
Your healthcare professional is likely to ask you a number of questions. Being ready to answer them may give you more time to discuss a concern in greater detail. Your health professional may ask:
- What symptoms have you been experiencing?
- When did you first notice them?
- Do you always have symptoms, or do they come and go?
- How severe are your symptoms?
- What, if anything, makes your symptoms better or worse?
- Has anyone in your family ever been diagnosed with liver disease?
- Do you have any chronic health conditions?
- Do you have a history of hepatitis or other liver disease?
- How much alcohol do you drink?
- What medicines are you taking?
- Do you take any herbal or natural remedies?
© 1998-2026 Mayo Foundation for Medical Education and Research(MFMER). All rights reserved. Terms of Use
