Sjogren syndrome
Conditions
Overview
Sjogren (SHOW-grin) syndrome is an ongoing, called chronic, condition of the immune system. It is also known as Sjogren disease. The two most common symptoms are dry eyes and a dry mouth.
In autoimmune conditions, the body attacks its own tissues by mistake. Sjogren syndrome most often affects the glands that make moisture in the eyes and mouth. This causes fewer tears and less saliva. The condition may happen with other immune system conditions, most often rheumatoid arthritis and lupus.
Sjogren syndrome can happen at any age. But most people are older than 40 at the time of diagnosis. The condition is much more common in people assigned female at birth. Treatment focuses on easing symptoms.
Symptoms
The two main symptoms of Sjogren syndrome are:
- Dry eyes. The eyes might burn or itch. They might feel as if they have sand in them.
- Dry mouth. The mouth might feel as if it's full of cotton. This may make it hard to swallow or speak.
Some people with Sjogren syndrome also have one or more of the following:
- Joint pain, swelling and stiffness.
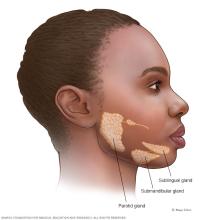
- Swelling of the glands that make saliva. This mainly affects the glands and in front of the ears.
- Skin rashes or dry skin.
- Dry vagina.
- Dry cough.
- Tiredness.
Causes
Experts don't know what causes the immune system to attack the body in Sjogren syndrome. Certain genes put people at higher risk of the condition. But it seems that an infection with a certain virus or strain of bacteria may bring it on.
Risk factors
Sjogren syndrome most often happens in people with one or more known risk factors, including:
- Age. Sjogren syndrome is mainly diagnosed in people older than 40.
- Sex. People assigned female at birth are much more likely to have Sjogren syndrome.
- Rheumatic disease. It's common for people who have Sjogren syndrome also to have a rheumatic disease, such as rheumatoid arthritis or lupus.
Complications
The most common complications of Sjogren syndrome involve the eyes and the mouth. These complications include:
- Dental cavities. Saliva helps protect the teeth from the germs that cause cavities. So a dry mouth is more likely to get cavities.
- Yeast infections. People with Sjogren syndrome are much more likely to get oral thrush, a yeast infection in the mouth.
- Vision issues. Dry eyes can lead to being sensitive to light and having blurred vision. Dry eyes also can damage the dome-shaped outer layer of the eye, called the cornea.
Less common complications might affect:
- Lungs, kidneys or liver. Swelling and irritation, called inflammation, can cause pneumonia, bronchitis or other issues in the lungs. Inflammation can keep the kidneys from working as they should and can cause the liver conditions hepatitis and cirrhosis.
- Lymph nodes. A small number of people with Sjogren syndrome get cancer of the lymph nodes. These are small, bean-shaped glands \that help fight infection. The cancer is called lymphoma.
- Nerves. Numbness, tingling and burning in the hands and feet might happen. This is called peripheral neuropathy.
Diagnosis
Diagnosis of Sjogren syndrome involves a physical exam and certain tests. Tests can help rule out other conditions and pinpoint a diagnosis of Sjogren syndrome.
Some medicines can cause dry mouth. These include medicines taken for allergies and depression. So your healthcare professional may do a review of the medicines you take.
Blood tests
Blood tests check for:
- Levels of certain types of blood cells.
- Antibodies common in Sjogren syndrome.
- Swelling and irritation, called inflammation.
- Issues with the liver and kidneys.
Eye tests
A test called a Schirmer tear test can measure eye dryness. A healthcare professional puts a small piece of filter paper under the lower eyelid to see how well the eyes make tears.
A specialist in eye conditions, called an ophthalmologist, also may look at the surface of the eyes with a magnifying device called a slit lamp. Drops put in the eye can make it easier to see damage to the dome-shaped outer layer of the eye, called the cornea.
Imaging
Certain imaging tests can check how well the glands that make saliva, called the salivary glands, work.
- Sialogram. This special X-ray can see dye that's put into the salivary glands in front of the ears. This shows how much saliva flows into the mouth.
- Salivary scintigraphy. This nuclear medicine test involves putting a radioactive isotope into a vein. The test tracks the isotope over an hour to see how fast it gets to the salivary glands.
Biopsy
A healthcare professional also may remove a small piece of tissue from the inside of the lower lip for study under a microscope. This is called a biopsy. It can find certain cells that might be a sign of Sjogren syndrome.
Treatment
Treatment for Sjogren syndrome depends on the parts of the body affected. Many people manage the dry eyes and dry mouth of Sjogren syndrome by using eye drops such as artificial tears and sipping water often. But some people need prescription medicines or surgical procedures.
Medications
Depending on your symptoms, your healthcare professional might suggest medicines that:
- Lessen eye swelling and irritation. Prescription eye drops such as cyclosporine (Restasis, Verkazia, others) or lifitegrast (Xiidra) can treat moderate to very dry eyes.
- Make more saliva. Medicines such as pilocarpine (Salagen) and cevimeline (Evoxac) can help make more saliva and sometimes more tears. Side effects can include sweating, belly pain, flushing and increased urination.
- Ease complications. If you get arthritis symptoms, a nonsteroidal anti-inflammatory drug, called NSAID, or other arthritis medicine might help. Antifungal medicines can treat yeast infections in the mouth.
- Treat symptoms that affect the whole body. Hydroxychloroquine (Plaquenil, Sovuna), a medicine to treat malaria, may help in treating Sjogren syndrome. So might medicines that lower immune response, such as methotrexate (Trexall).
Surgery
A minor procedure to seal the tear ducts that drain tears from the eyes, called punctal occlusion, may help ease dry eyes. Collagen or silicone plugs placed in the ducts help save tears.
Lifestyle and home remedies
Many Sjogren syndrome symptoms respond well to self-care measures.
To ease dry eyes:
-
Use artificial tears, an eye lubricant or both. Commonly called eye drops, artificial tears may ease dry eyes.
You don't have to use eye lubricants as often as artificial tears. But because eye lubricants are thicker, they can blur your vision. So you might want to use them only before bedtime.
You may need to use artificial tears without preservatives if preservatives irritate your eyes.
- Raise humidity. Raise the humidity indoors by using a humidifier. And don't let air blow into your face. For instance, don't sit in front of a fan or air conditioning vent. Wear goggles or eyewear that protects your eyes when you go outdoors.
To help with dry mouth:
- Don't smoke. Smoking can irritate and dry out your mouth.
- Drink more fluids. Take sips of fluids, mainly water, throughout the day. Don't drink coffee or alcohol, which can dry your mouth more. Also don't drink beverages such as colas and some sports drinks because the acid can harm the coating of your teeth.
- Make more saliva. Sugarless gum or citrus-flavored hard candies can help with saliva flow. Because Sjogren syndrome increases your risk of dental cavities, limit sweets. Don't eat sweets between meals.
- Try artificial saliva. Saliva replacement products often work better than plain water because they have a lubricant that helps your mouth stay moist longer. These products come as a spray or lozenge.
- Use nasal saline spray. A nasal saline spray can help moisturize and clear nasal passages so that you can breathe freely through your nose. A dry, stuffy nose can make mouth breathing more likely. Mouth breathing increases mouth dryness.
Oral health
Dry mouth increases your risk of dental cavities and tooth loss. To help prevent those types of issues:
- Brush your teeth and floss after every meal.
- Make dental appointments at least every six months.
- Use daily topical fluoride treatments and antimicrobial mouthwashes.
Other areas of dryness
If dry skin is a problem, don't bathe or shower in hot water. Pat your skin with a towel to dry off. Don't rub. Put moisturizer on when your skin is still damp. Use moisturizer made for extra dry skin.
Use rubber gloves when washing dishes or housecleaning. Vaginal moisturizers and lubricants can help vaginal dryness. Lip balm can help dry lips.
Preparing for an appointment
Depending on your symptoms, you might start by seeing your family healthcare professional, dentist or eye doctor. In time, you might see a doctor who specializes in the treatment of arthritis and other inflammatory conditions, called a rheumatologist.
What you can do
Make a list that includes:
- Your symptoms and when they began.
- Other medical conditions you have.
- Your and your families' medical histories.
- All medicines, vitamins or supplements you take, including dosages.
- Questions to ask your healthcare professional.
For Sjogren syndrome, basic questions include:
- What is likely causing my symptoms?
- What are other possible causes?
- What tests do I need?
- What treatment do you suggest?
- How soon can I expect my symptoms to get better with treatment?
- Am I at risk of long-term complications from this condition?
- I have other health conditions. How can I best manage them together?
- Do you have brochures or other printed materials that I can have? What websites do you suggest?
What to expect from your doctor
Your healthcare professional is likely to ask you questions, including:
- Do your symptoms follow a pattern, such as getting worse throughout the day or when you go outdoors?
- Do you have lasting conditions such as high blood pressure or arthritis?
- Have you recently started new medicines?
- Do any close relatives have rheumatoid arthritis, lupus or a similar condition?
© 1998-2026 Mayo Foundation for Medical Education and Research(MFMER). All rights reserved. Terms of Use
