Viral hepatitis
Conditions
Overview
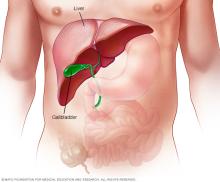
Hepatitis is swelling of the liver, called inflammation, often caused by an infection. When a virus causes hepatitis, it's called viral hepatitis. There are five different types of the hepatitis virus, named A, B, C, D and E. Other viruses that can affect the liver include the viruses that cause chickenpox and mononucleosis.
The five hepatitis viruses are spread in different ways and can cause different symptoms. Many people may not know they have hepatitis because they don't have symptoms.
Screening, early testing and treatment may help lower the risks of some hepatitis viruses and the risk of serious liver damage such as cirrhosis, liver failure or liver cancer.
Vaccines can prevent hepatitis strains A and B. A hepatitis B vaccine prevents hepatitis D. A hepatitis E vaccine only is available in parts of Asia. Hepatitis C currently has no vaccine available.
Hepatitis also can be caused by certain bacteria, medicines, chemicals, health conditions and alcohol.
Types
The five hepatitis viruses are A, B, C, D and E. These viruses primarily infect liver cells. The main problem they cause is inflammation of the liver, known as hepatitis. They are described as hepatotropic, meaning they have a preference for infecting the liver.
Some other viruses, like cytomegalovirus and the Epstein-Barr virus, can infect many parts of your body. The liver usually isn't the target. The medical term for this is nonhepatotropic.
Viral hepatitis viruses cause infections that are acute or chronic:
- Acute infections are short-term and last less than six months. The body's immune system kills the hepatitis virus and makes antibodies to help protect against future infection.
- Chronic infections are long-term and last more than six months. The virus weakens the body's immune system. The cells that typically kill the hepatitis virus aren't effective. As a result, the virus stays in the body.
Hepatitis A
The hepatitis A virus causes an acute infection. Worldwide, hepatitis A is the most common cause of acute viral hepatitis. If you get a hepatitis A infection, your body builds immunity. You can't get another hepatitis A infection in the future. But a relapse right after recovery from an infection is possible.
Hepatitis B
The hepatitis B virus causes acute and chronic infections. Hepatitis B flares in chronic infections are common. A flare is a sudden increase in an enzyme found in the liver that helps convert proteins into energy for the liver cells. Flares can occur for several reasons such as during antiviral treatment, interferon treatment or immunosuppressive treatment. Flares that occur for no known reason are called spontaneous flares. Chronic hepatitis B has no cure but can be managed.
Hepatitis C
The hepatitis C virus causes acute and chronic infections. Hepatitis C infections are mostly chronic. Many people who have hepatitis C don't know that they have it. Hepatitis C can be cured. But another hepatitis C infection in the future is possible.
Hepatitis D
The hepatitis D virus causes acute and chronic infections. The hepatitis D virus needs the hepatitis B virus to make someone sick. Worldwide, hepatitis D is the most severe form of viral hepatitis. Hepatitis D and B infections can happen at the same time, called coinfection. A hepatitis D infection can occur in someone who has chronic hepatitis B, called superinfection. Hepatitis D infection is mostly acute. Rarely, it can become chronic. If you have immunity to hepatitis B, you're protected from a hepatitis D infection.
Hepatitis E
The hepatitis E virus causes acute and chronic infections. Worldwide, hepatitis E is one of the most common causes of acute viral hepatitis. If you get a hepatitis E infection, your body builds immunity that can last for several years. Chronic hepatitis E mostly affects people who have solid organ transplants or weakened immune systems. Chronic hepatitis E may be able to be cured.
Other types of hepatitis
Hepatitis can be caused by things other than viral hepatitis viruses:
- Other viruses. This can include infection with cytomegalovirus, the herpes simplex virus, and the Epstein-Barr virus, which causes mononucleosis. The varicella zoster virus, which causes chickenpox and shingles, also can cause liver damage.
- Certain bacteria. This can include infections with bacteria such as salmonella, campylobacter, listeria, legionella and the borrelia bacteria which causes Lyme disease.
- Complications of other conditions. Hepatitis can be caused by some autoimmune diseases such as metabolic dysfunction-associated steatotic liver disease (MASLD) or autoimmune hepatitis. Hepatitis can be caused by some conditions passed down through families, such as Wilson's disease or hemochromatosis.
Certain medicines and toxins can cause hepatitis and liver damage:
- Alcohol. Heavy alcohol use over many years can lead to hepatitis.
- Prescription medicines. This can include some medicines to treat high cholesterol, high blood pressure, seizures and cancer. Some antibiotics also may damage the liver.
- Pain relief medicines. Some pain relief medicines you can buy without a prescription can cause toxic hepatitis. Medicines such as acetaminophen (Tylenol, others), ibuprofen (Advil, Motrin IB, other) or aspirin can damage the liver, especially if taken often or combined with alcohol.
- Herbs and supplements. Some herbs considered dangerous to the liver include aloe vera, black cohosh, chaparral, garcinia cambogia, germander, kava and turmeric. There are many others.
- Industrial chemicals. Chemicals you may be exposed to on the job can cause liver injury. Common chemicals that can cause liver damage include the dry cleaning solvent carbon tetrachloride and a substance called vinyl chloride that's used to make plastics. The herbicide paraquat and a group of industrial chemicals called polychlorinated biphenyls also may damage the liver.
Symptoms
Symptoms of hepatitis viruses vary. Some people have mild symptoms. Others have severe symptoms. Some people have no symptoms.
Common symptoms of hepatitis A, B, C, D and E infections include:
- Feeling tired and weak.
- Fever.
- Not wanting to eat.
- Joint pain.
- Dark-colored urine.
- Yellowing of the skin and the white of the eyes, called jaundice. Yellowing of the skin might be harder to see on some skin colors.
- Belly pain, especially on the upper right side under your lower ribs, which is over your liver.
- Upset stomach, throwing up.
Other symptoms may include:
- Clay- or gray-colored stools. This is common to hepatitis A, D and E viruses.
- Sudden diarrhea or intense itching. These are common to hepatitis A. Itching also is common to hepatitis E.
- Bruising easily, itchy skin, fluid buildup in the stomach, swelling in the legs, confusion, drowsiness and slurred speech. This is common to hepatitis C.
- Skin rash. This is common to hepatitis E.
When symptoms typically appear
Symptoms appear after the hepatitis virus enters the body:
| Hepatitis type | Time from infection to symptoms | |||
|---|---|---|---|---|
| Hepatitis A | 2 to 6 weeks. | |||
| Hepatitis B | 4 to 24 weeks. | |||
| Hepatitis C | 7 to 8 weeks. | |||
| Hepatitis D | About 3 weeks when hepatitis D and hepatitis B infections occur at the same time. This is known as a coinfection. Symptoms start in 2 to 8 weeks when hepatitis D occurs in someone who has chronic hepatitis B. This is known as a superinfection. Symptoms are often more severe with superinfection. | |||
| Hepatitis E | 2 to 10 weeks. Symptoms most often start in 5 to 6 weeks. | |||
| Based on Wing EJ, et al., eds. Cecil Essentials of Medicine. 10th ed. Elsevier; 2022; Ferri FF. Ferri's Clinical Advisor 2026. Elsevier; 2026; World Health Organization. https://www.who.int/news-room/fact-sheets/detail/hepatitis-e. Accessed Jan. 9, 2026. Accessed Jan. 15, 2026; Minnesota Department of Health. https://www.health.state.mn.us/diseases/hepatitis/hepdfact.html. Accessed Jan. 20, 2026; Centers for Disease Control and Prevention. https://www.cdc.gov/hepatitis-d/about/index.html. Accessed Feb. 2, 2026. | ||||
When to see a doctor
See a healthcare professional if you:
- Have any symptoms of hepatitis.
- Know you've been exposed to a hepatitis virus. You may have mild symptoms or no symptoms and still be infected.
Seek emergency care if you have these symptoms of acute liver failure:
- Sudden yellowing of the eyes or skin.
- Tenderness in the upper belly.
- Any unusual changes in mental state, personality or behavior.
Acute liver failure is a condition in which the vital functions of the liver quickly shut down. It's a medical emergency.
Causes
A common cause of hepatitis is a hepatitis virus:
Hepatitis A
The hepatitis A virus spreads when tiny amounts of infected stool get into another person's mouth. You can get an infection if you:
- Eat food handled by someone with the virus who doesn't wash their hands well after using the toilet.
- Drink contaminated water or eat food washed in contaminated water.
- Have sexual contact or close contact with someone who has the hepatitis A virus.
Children and adults can become infected.
Hepatitis B and C
The hepatitis B and C viruses spread through contact with blood, body fluids or needles that have the virus in it. You can get a hepatitis B or C infection if you:
- Have sex with someone who has hepatitis B or C and a condom isn't used.
- Come into contact with infected blood or body fluids, such as saliva, semen or vaginal fluids.
- Share needles to inject illegal drugs.
- Use unclean equipment for tattoos or piercings.
The virus also can be passed from pregnant people to their babies during childbirth. Children and adults can become infected. But hepatitis C virus infection is more common among adults than children.
Hepatitis D
The hepatitis D virus only occurs in someone who is infected by the hepatitis B virus. You can get an infection if you:
- Have sex with someone who has hepatitis B and a condom isn't used.
- Come into contact with infected blood or body fluids, such as saliva, semen or vaginal fluids.
- Share needles to inject illegal drugs.
The virus also can be passed from pregnant people to their babies during childbirth. Children and adults can become infected. The infection is often more serious among children and people who use illegal drugs who also have hepatitis C.
Hepatitis E
The hepatitis E virus spreads when tiny amounts of infected stool get into another person's mouth. You can get an infection if you:
- Eat food handled by someone with the virus who doesn't wash their hands well after using the toilet.
- Drink contaminated water or eat food washed in contaminated water.
- Eat undercooked meats such as pigs and deer, undercooked shellfish or vegetables grown with contaminated water.
Hepatitis E virus infection is more common among adults than children.
How hepatitis viruses aren't spread
Hepatitis viruses can't be spread by sharing food and eating utensils, and kissing or hugging someone with a hepatitis virus. Hepatitis viruses also can't be spread by coughing or sneezing.
Risk factors
Hepatitis A
Your risk of getting hepatitis A is higher if you:
- Travel, live or work in areas of the world where hepatitis A is common. This includes places with poor sanitation and unsafe water.
- Live with someone who has hepatitis A. Live in or work at a group home or work at a child care center.
- Have any type of sexual contact with someone who has hepatitis A. Are assigned male at birth and have sex with others assigned male at birth.
- Have HIV.
- Use recreational drugs, even if they aren't injected.
Hepatitis B
Your risk of getting hepatitis B is higher if you:
- Have sex without a condom with multiple partners or with someone who's infected with hepatitis B.
- Share syringes or needles to inject drugs or use unclean equipment for tattoos or body piercings.
- Are assigned male at birth and have sex with others assigned male at birth.
- Live with someone who has a chronic hepatitis B infection.
- Were born to a pregnant person who had hepatitis B.
- Have a job that involves contact with human blood.
- Have hepatitis C or HIV.
If you're at an increased risk of getting hepatitis B, your healthcare professional may want to test you for hepatitis B. This is called screening. Screening is important because the hepatitis B virus can damage the liver before the hepatitis B symptoms start. If you have not been vaccinated, your healthcare professional may want to vaccinate you for hepatitis B.
Hepatitis C
Your risk of getting hepatitis C is higher if you:
- Share syringes or needles to inject drugs or use unclean equipment for tattoos or body piercings.
- Received donated blood or a solid organ transplant before 1992.
- Have had long-term hemodialysis.
- Are a healthcare and emergency worker who has contact with blood or been stuck by a needle.
- Have hemophilia and were treated with clotting factors before 1987.
Also, your risk of getting hepatitis C is higher if you:
- Have been in prison.
- Were born to a pregnant person who has a high viral load of hepatitis C.
- Have sex without a condom with multiple partners or with someone who's infected with hepatitis C.
- Are assigned male at birth and have sex with others assigned male at birth.
- Have HIV.
If you're at an increased risk of getting hepatitis C, your healthcare professional may want to test you for hepatitis C. This is called screening. All adults ages 18 to 79 years are recommended to have hepatitis C screening, including pregnant people.
Hepatitis D
Your risk of getting hepatitis D is higher if you:
- Have a hepatitis B infection.
- Live with someone who has a chronic hepatitis B or hepatitis D infection.
- Travel, live or work in areas of the world where hepatitis B is common.
- Have a job that involves contact with human blood.
- Have sex without a condom with multiple partners or with someone who's infected with hepatitis B.
- Share syringes or needles to inject drugs or use unclean equipment for tattoos or body piercings.
Also, your risk of getting hepatitis D is higher if you:
- Are assigned male at birth and have sex with others assigned male at birth.
- Were born to a pregnant person who had hepatitis B or D.
- Have HIV.
Hepatitis E
Your risk of getting hepatitis E is higher if you:
- Travel, live or work in places with poor sanitation and unsafe water.
- Had one or more solid organ transplants of your heart, liver, kidney, lung or pancreas.
- Have HIV.
- Have a blood cancer such as non-Hodgkin lymphoma and lymphoplasmacytic lymphoma.
- Have rheumatological diseases such as rheumatoid arthritis, psoriatic arthritis and lupus.
- Were born to a pregnant person who had hepatitis E.
Complications
Hepatitis can cause serious liver damage such as advanced scarring of the liver, called cirrhosis, or the buildup of scar tissue over areas of swelling or injury, called fibrosis. Liver cancer and acute liver failure also are possible complications of severe liver damage.
Hepatitis A
In rare cases, hepatitis A can cause acute liver failure, especially in older adults or people with chronic liver diseases. Some people with acute liver failure may need a liver transplant. Hepatitis A typically doesn't cause long-term liver damage.
Hepatitis A also can cause arthritis, and swelling of small blood vessels, known as leukocytoclastic vasculitis. The swelling can cause red, purple or brownish-yellow blotches or bumps that can appear on or under the skin.
Hepatitis B
- Acute infection. In rare cases, an acute hepatitis B infection can cause acute liver failure.
- Chronic infection. A chronic hepatitis B infection can cause cirrhosis or liver cancer. In some people, levels of the virus are low or haven't yet been found by tests. If the virus starts to quickly make copies of itself, tests may spot this rise or find the virus. This is called reactivation of the virus. It can lead to liver damage or even liver failure. Reactivation tends to affect people who have weakened immune systems. This includes people on medicines that weaken the immune system, such as high-dose corticosteroids, glucocorticoids or chemotherapy.
Hepatitis C
- Acute infection. An acute hepatitis C infection can lead to a chronic infection.
-
Chronic infection. A chronic hepatitis C infection can cause fibrosis, cirrhosis and liver cancer. Some people with cirrhosis may need a liver transplant. Rarely, a chronic infection can cause B-cell non-Hodgkin lymphoma.
The virus can cause several other health conditions such as swelling of blood vessels, known as cryoglobulinemia, and a rash, known as lichen planus. The rash appears as purple, red, brown or gray. The shiny, flat bumps are often found on the inner forearms, wrists or ankles. The rash can cause itching. Lacy white patches can form on the tongue or inside of the cheeks.
Hepatitis D
- Acute infection. An acute hepatitis D infection that occurs with a hepatitis B infection can cause acute liver failure. An acute hepatitis D infection that occurs in someone who has chronic hepatitis B can turn into a chronic hepatitis D infection or chronic liver failure.
- Chronic infection. A chronic hepatitis D infection can cause acute liver failure, fibrosis, cirrhosis and liver cancer. Some people with acute liver failure may need a liver transplant.
Hepatitis E
-
Acute infection. Rarely, an acute hepatitis E infection can cause serious problems in pregnant people, especially during the second and third trimesters. Risks include acute liver failure, which requires a stay in the hospital for monitoring and treatment. Some people with acute liver failure may need a liver transplant.
An acute hepatitis E infection can become a chronic infection in people who have solid organ transplants, weakened immune systems, HIV, arthritis and rheumatic diseases, or cancers of the blood. Hepatitis E can affect other areas of the body such as the pancreas, thyroid, kidneys and heart.
- Chronic infection. A chronic infection can lead to liver fibrosis and cirrhosis in people who have solid organ transplants or weakened immune systems. Hepatitis E also can cause liver failure and acute liver failure.
Prevention
Hepatitis A
The best way to protect yourself from a hepatitis A infection is to get the hepatitis A vaccine. Talk with your healthcare professional if you're planning international travel and you aren't sure if you've been vaccinated.
The vaccine is typically given in two shots. The first shot is followed by a booster shot six months later. The hepatitis A vaccine can be given in a combination that includes the hepatitis B vaccine. This vaccine combination is given in three shots over six months.
Other ways you can protect yourself include:
- Wash your hands with soap and water. The hepatitis A virus can stay on fingers for up to four hours. The virus can live on indoor surfaces and in food, water or soil for months. Wash your hands often, especially after using the toilet or changing a diaper and before and after preparing food or eating. Help make sure your children wash their hands with soap and water. Baby wipes don't remove germs.
-
Follow food safety guidelines when you travel. If you travel to an area that has a hepatitis A outbreak, take extra precaution. Make sure meats are cooked thoroughly and are hot. Don't eat raw or undercooked meat, fish and shellfish. Wash all fresh fruits and vegetables in bottled water and peel them yourself.
Use bottled water to drink and when you brush your teeth. Avoid all beverages if you don't know if they contain tap water. The same goes for ice. If bottled water isn't available, boil tap water before using.
Hepatitis B, C and D
The best way to protect yourself from a hepatitis B and D infection is to get the hepatitis B vaccine. But the hepatitis B vaccine won't protect you from hepatitis D if you already have chronic hepatitis B.
The hepatitis B vaccine is given as two shots one month apart, or three or four shots over six months. How many shots you get depends on the type of hepatitis B vaccine that you're given. Talk with your healthcare professional if you're planning international travel and you aren't sure if you've been vaccinated.
There are no vaccines to prevent hepatitis C or D.
Other ways you can protect yourself include:
- Practice safer sex. Use a new latex or polyurethane condom correctly every time you have sex if you don't know the health status of your partner. Condoms can lower your risk of catching hepatitis, but they don't get rid of the risk completely.
- Don't use illegal drugs. If you use drugs, get help to stop. If you can't stop, use a sterile needle each time you inject drugs. Never share needles and equipment.
- Be careful about body piercing and tattooing. If you want to get a piercing or tattoo, look for a reputable shop that is regulated. Ask about how the equipment is cleaned. Make sure the employees use sterile needles. If you can't get answers, look for another shop.
- Don't share personal items. Viruses can spread if infected blood or body fluids come into contact with the eyes, nose or mouth. They also can enter the body through cuts or scrapes in the skin. Don't share or use items that have blood on them such as razors, toothbrushes, toys and medical equipment. Clean up any blood spill with bleach or detergent. Wear single-use gloves.
Hepatitis E
There is no vaccine for hepatitis E in North America. Ways to protect yourself include:
- Follow food safety guidelines when you travel. If you travel to an area that has a hepatitis E outbreak, take extra precaution. Make sure meats are cooked thoroughly and are hot. Don't eat raw or undercooked pork or meat, shellfish and wild animal meats. Avoid food from street vendors.
- Follow water safety guidelines when you travel. The hepatitis E virus can live in water for many weeks. Use bottled water to drink and when you brush your teeth. Avoid all beverages if you don't know if they contain tap water. The same goes for ice. If bottled water isn't available, boil tap water before using. Wash all fresh fruits and vegetables in bottled water and peel them yourself.
- Wash your hands with soap and water. The hepatitis E virus can live on surfaces such as plastic, wood and stainless steel at room temperature for a few weeks. The virus survives longer at lower temperatures. Wash your hands often, especially after using the toilet or changing a diaper and before and after preparing food or eating. Help make sure your children wash their hands with soap and water. Baby wipes don't remove germs.
Diagnosis
Your healthcare professional may give you a physical exam and look for symptoms of liver damage such as yellowing skin and stomach pain. Different blood tests can detect all five types of hepatitis viruses. A sample of blood is taken, usually from a vein in your arm. The sample is sent to a laboratory for testing.
Hepatitis A
Blood test results can tell your healthcare professional if the infection is current or if you had a hepatitis A infection in the past.
Hepatitis B
Blood test results can tell your healthcare professional if the infection is acute or chronic.
Tests that check for liver damage or complications caused by hepatitis B include:
- Transient elastography. This imaging test is a type of ultrasound that sends vibrations into the liver. The test measures how fast the vibrations go through liver tissue. It shows places where the liver is stiff.
- Magnetic resonance elastography (MRE). This test combines magnetic resonance imaging (MRI) with low-frequency vibrations to create a visual map that shows areas of liver stiffness.
- Liver biopsy. A small sample of liver tissue is removed using a thin needle and sent to a lab to check for damage. This is called a liver biopsy.
Hepatitis C
Blood test results can tell your healthcare professional if the infection is current or if you had a hepatitis C infection in the past. Blood tests also can:
- Measure the quantity of the hepatitis C virus in your blood, called the viral load.
- Identify the genotype and subtype of the virus to help guide treatment.
- Evaluate the health of your liver.
Tests that check for liver damage or complications caused by hepatitis C are similar to those used for hepatitis B. These may include transient elastography, magnetic resonance elastography (MRE) or liver biopsy.
Hepatitis D
Blood test results can tell your healthcare professional if the infection is current or you had a hepatitis D infection in the past.
Hepatitis E
Blood test results can tell your healthcare professional if the infection is current, near the end of recovery or if an infection occurred in the past. Stool tests also can detect the hepatitis E virus.
Treatment
Hepatitis A
No specific treatment exists for hepatitis A. The body clears the hepatitis A virus on its own. In most cases, the liver heals within six months with no lasting damage.
Getting the hepatitis A vaccine or an injection of an antibody called immunoglobulin within two weeks of exposure to the hepatitis A virus may protect you from infection.
Hepatitis B
Acute hepatitis B infection treatment typically isn't needed. The infection often goes away on its own.
Chronic hepatitis B infection treatment typically focuses on lowering the risk of liver damage such as cirrhosis and liver cancer, and improving long-term survival. Chronic hepatitis B can't be cured.
Most people with chronic hepatitis B virus infection need treatment for the rest of their lives. The decision to start treatment depends on many factors, including how much damage your liver has from fibrosis or cirrhosis and if you have other infections such as HIV.
Treatment for chronic hepatitis B may include:
- Antiviral medicines. Many antiviral medicines can help fight the virus and slow its ability to damage your liver. Entecavir (Baraclude) and tenofovir (Viread) are the two most common medicines prescribed. Your healthcare professional may prescribe lamivudine (Epivir) or adefovir (Hepsera). You take antiviral medicines by mouth, most often for the long term. Antiviral medicines are safe for people who are pregnant.
-
Interferon shots. Interferon is a lab-made version of a substance that the body makes to fight infection. This type of medicine includes peginterferon alfa-2a (Pegasys). One upside of interferon shots is that they're taken for a much shorter time than are antiviral medicines. But interferon has a high rate of side effects, such as upset stomach, vomiting, trouble breathing and depression.
Interferon mainly is used for young people with hepatitis B who wish to not need long-term treatment. It's also used for people who might want to get pregnant within a few years. Do not take interferon during pregnancy. Interferon also may be unsafe for people with cirrhosis or acute liver failure.
- Liver transplant. If your liver has been badly damaged, a liver transplant may be an option. During a liver transplant, the surgeon removes your damaged liver and replaces it with a healthy liver. The new liver may come from a donor who has died or from a living person who donates part of the liver.
Getting the hepatitis B vaccine, an injection of an antibody called immunoglobulin, or both after exposure to the hepatitis B virus may protect you from infection.
Hepatitis C
Blood tests can't tell the difference between an acute or chronic hepatitis C infection. Acute infections can go away on their own but most often hepatitis C infections are chronic.
Hepatitis C infection treatment focuses on clearing the virus from the body and lowering the risk of chronic liver disease. Treatment is typically given whether the infection is acute or chronic. Hepatitis C can be cured.
Treatment for hepatitis C may include:
-
Antiviral medicines. Antiviral medicines focus on clearing the virus from the body for at least 12 weeks after treatment ends. Some newer antiviral medicines, called direct-acting, have better outcomes, fewer side effects and shorter treatment times. Treatment can be as short as eight weeks.
The choice of medicines and length of treatment depend on the hepatitis C genotype, whether the liver is damaged, other medical conditions and earlier treatments. Throughout treatment, the care team watches the treatment for response to the medicines and side effects. Treatment with direct-acting antiviral medicines usually lasts 12 weeks.
-
Liver transplant. A liver transplant might be an option for serious liver damage from chronic hepatitis C infection. During a liver transplant, a surgeon removes the damaged liver and replaces it with a healthy liver. Most transplanted livers come from dead donors. A small number come from living donors who donate a part of their livers.
In most cases, a liver transplant alone doesn't cure hepatitis C. The infection is likely to return. This means more treatment with antiviral medicines to prevent damage to the new liver. Studies have shown that newer antiviral medicines cure hepatitis C after a transplant.
Hepatitis D
Acute hepatitis D infection treatment typically isn't needed. The infection is short lived and most often it goes away on its own.
Chronic hepatitis D infection treatment typically focuses on lowering the risk of liver damage such as cirrhosis and liver cancer, and improving long-term survival. People who have a superinfection with a chronic hepatitis B infection are sicker than people who have a coinfection with hepatitis B. Chronic hepatitis D can't be cured.
Treatment for hepatitis D may include:
- Interferon shots. Interferon is a lab-made version of a substance that the body makes to fight infection. This type of medicine includes peginterferon alfa-2a (Pegasys). Interferon has a high rate of side effects and relapses. Interferon shots are typically given for one year or longer. Do not take interferon during pregnancy. Interferon also may be unsafe for people with cirrhosis or acute liver failure.
- Liver transplant. If your liver has been badly damaged, a liver transplant may be an option. During a liver transplant, the surgeon removes your damaged liver and replaces it with a healthy liver. The new liver may come from a donor who has died or from a living person who donates part of the liver.
- New medicines. Researchers are working on new medicines to help treat chronic hepatitis D infections.
Hepatitis E
Acute hepatitis E infection treatment typically isn't needed. The infection often goes away on its own.
Chronic hepatitis E infection typically affects people who have weakened immune systems caused by solid organ transplants, some types of chemotherapy or illnesses such as HIV. Treatment focuses on reducing risks such as liver fibrosis and cirrhosis. Chronic hepatitis E may be able to be cured.
Treatment for hepatitis E may include:
- Reducing immunosuppressant medicines. A person who receives a solid organ transplant needs to take medicines to prevent organ rejection. Reducing the medicine helps the immune system fight the hepatitis E infection. Your healthcare team monitors your transplanted organ for signs of rejection.
-
Antiviral medicine. Ribavirin (Virazone and Ribasphere) is an antiviral medicine used to help fight the virus and slow its ability to damage your liver. You take ribavirin by mouth, most often every day for three months. The most common side effect of ribavirin is anemia that may need blood transfusions or injections of erythropoietin, a lab-made version of a substance that helps the body make red blood cells. Do not take ribavirin during pregnancy.
Your healthcare professional may recommend a second treatment of ribavirin. Or you may take ribavirin with interferon to improve treatment response.
- Interferon shots. Interferon is a lab-made version of a substance that the body makes to fight infection. This type of medicine includes peginterferon alfa-2a (Pegasys). Interferon has a high rate of side effects and relapses. Interferon raises the risk of sudden organ rejection in people who have an organ transplant.
Lifestyle and home remedies
Help manage hepatitis symptoms with self-care measures:
- Rest. Many people with hepatitis feel tired and sick and have less energy.
- Eat well. Eat a balanced healthy diet. Nausea can make it difficult to eat. Try snacking throughout the day rather than eating full meals. To get enough calories, eat more high-calorie foods.
- Drink liquids to stay hydrated. It's important to prevent dehydration, especially if you have vomiting or diarrhea.
- Avoid alcohol. Don't drink alcohol. It can cause liver damage.
- Use medicines with care. Your liver may have a hard time processing some medicines. Talk with your healthcare professional about all the medicines you take, including medicines you can buy without a prescription.
Preparing for an appointment
If you have been exposed to hepatitis or have symptoms of hepatitis, make an appointment with your healthcare professional. Preparing and anticipating questions can help you make the most of your appointment.
What you can do
Because appointments can be brief and there's often a lot of information to cover, it's a good idea to be prepared.
- Be aware of pre-appointment restrictions. When you make the appointment, find out if there's anything you need to do in advance, such as change your diet.
- Make a list of your symptoms. Include those that seem unrelated to the reason for your appointment.
- Make a list of key personal information, including major stresses or recent life changes and recent travel or possible exposure to hepatitis.
- Make a list of all medicines, vitamins, herbs and other supplements you take. List how much you take of each one.
- Consider bringing a family member or friend. Someone who goes with you may remember something that you missed or forgot.
- Prepare a list of questions to ask your healthcare professional.
Basic questions to ask
Some basic questions to ask include the following.
Causes and diagnosis
- What is likely causing my symptoms or condition?
- What are other possible causes?
- What tests do I need? Should I be tested for other causes of liver disease?
- Is my condition likely short term or long term?
Treatment and overall health
- Do I need treatment for a hepatitis infection?
- What treatment choices do I have? What are the benefits and risks of each treatment choice?
- Are there any other treatment choices besides the one you suggest?
- Is there a generic version of the medicine you're prescribing?
- I have other health conditions. How can I best manage them together?
- Are there restrictions that I need to follow, including alcohol or medicines to avoid?
Protecting others and daily life
- Can I pass hepatitis to others? How can I protect people around me?
- Should my family be tested?
- Is there a vaccine for the type of hepatitis I have? If there is, should people close to me receive the hepatitis vaccine?
- If someone close to me is diagnosed with hepatitis, is there a vaccine to prevent infection?
- Can I continue to work or go to school?
- How will I know when I can no longer spread hepatitis?
- What symptoms could signal serious complications?
More information and care
- Should I see a specialist?
- Are there brochures or websites you recommend?
What to expect from your doctor
Your healthcare professional may ask you questions such as the following.
Possible exposure
- Have you recently traveled or been in an area with contaminated water or a hepatitis outbreak?
- Have you been exposed to someone with hepatitis?
- Have you been vaccinated for hepatitis A or B?
- Have you had hepatitis before?
Symptoms
- When did your symptoms begin?
- Are your symptoms constant or do they come and go?
- How bad are your symptoms?
- What, if anything, makes your symptoms better?
- What, if anything, makes your symptoms worse?
Symptoms and past diagnosis questions if hepatitis B or C is suspected include:
- Have you had jaundice, such as yellowing of the eyes or light-colored stool?
- Have you been diagnosed with hepatitis or another liver condition?
- Have you ever had a blood transfusion or organ transplant?
- Do you inject drugs?
- Have you had sex without a condom?
- How many sexual partners have you had?
- Does anyone in your family have hepatitis or liver disease?
© 1998-2026 Mayo Foundation for Medical Education and Research(MFMER). All rights reserved. Terms of Use
